Learning Objectives
This is an intermediate level course. After completing this
course, mental health professionals will be able to:
- Describe the nature of defiant, oppositional, or noncompliant behavior
in children.
- Explain the four major factors that contribute to such behavior,
known as the four-factor model of defiant behavior.
- Discuss the implications of this model for evaluating children
with this behavior pattern.
- Present the implications of this model for treatment of children
with ODD.
This course is largely adapted from Dr. Barkley’s book, Defiant Children: A Clinician’s Manual for Assessment and Parent Training. New
York: Guilford Press, 2013 (3rd ed.) It has been adapted with permission of the publisher.
The materials in this course are based on the most accurate
information available to the author at the time of writing. The scientific
literature on childhood defiant behavior and ODD grows daily, and new
information may emerge that supersedes these course materials. This course
material will equip clinicians to have a basic understanding of the nature,
assessment, and treatment of ODD in children. Readers are directed to the book for detailed information on how to implement Dr. Barkley's parent training program for the management of ODD in children.
Noncompliance/Defiance Defined
The term
“noncompliance” as used here will refer to three categories of child behavior,
these being the following:
- The child’s
failure to initiate behaviors requested by an adult within a reasonable time
after a command given by that adult. In most cases, a reasonable time refers to
15 seconds after the command was given, although parents may specifically
stipulate when compliance is to be initiated (e.g., “As soon as that cartoon is
over, pick up your toys!”). Research on noncompliance has generally used a more
stringent interval of 10 seconds after a command was given as a reasonable time
for compliance to be initiated.
- The child’s
failure to sustain compliance to a command from an adult until the requirements
stipulated in the command have been fulfilled. Some may consider this behavior
category as a form of attention span or sustained attention to tasks (“on-task”
behavior).
- The child’s
failure to follow previously taught rules of conduct in a situation. Such
behaviors as leaving one’s desk in class or running off in a department store
without permission, stealing, lying, hitting or aggressing against others,
taking food from the kitchen without permission, and swearing at one’s parents
are just a few child behaviors that parents consider to be violations of
previously taught standards of conduct.
The term
“noncompliance,” however, may convey the notion of passive avoidance of
completing parental commands and requests or following previously stated
household rules. Thus, the term “defiance” can also be used for many instances
of noncompliant behavior where the child not only fails to obey a directive or
rule, but also displays active verbal or physical resistance to complying with
such parental directives. This is an active resistance to direction rather than
a passive one as might be conveyed by the term noncompliance. For instance, as
when a child engages in verbal refusal, temper outbursts, and even physically
aggressing against a parent when the parent attempts to impose compliance with
a directive on the child. Examples of noncompliant behavior are:
Yells |
Steals |
Fails to
complete chores |
Whines |
Lies |
Destroys
property |
Complains |
Argues |
Physically
fights |
Defies |
Humiliates/Annoys |
Fails to do
school homework |
Cries or holds
breath |
Teases |
Disrupts
others activities |
Tantrums or
screams |
Ignores
requests |
Ignores
self-care routines |
Throws objects |
Self-injury |
Runs off |
Argues or
sarcastic |
Swears |
Physically
resists |
Despite their
apparent dissimilarity, all of these behaviors can be construed as belonging to
a more general or larger class of behavior that involves noncompliance. This
broad band of inter-related forms of behavior has also been termed “externalizing”
or “disruptive” behavior disorders and may include oppositional-defiant
disorder, hostile-defiant behavior, social aggression, or conduct or other
externalizing problems. Some of the behaviors in the list above are in fact
direct efforts of the child to escape or avoid the imposition of the command. Hence, all may be treated by a common program that
addresses noncompliance. Research has shown that treating noncompliance often
results in significant improvements in other behaviors in this general class
even though those behaviors were not specifically targeted by the intervention.
It is this targeting of noncompliance that distinguishes this parent training
program from many others, which may single out one or several types of
inappropriate behavior but fail to address the more general class of
noncompliance or defiance to which such specific forms of externalizing
behavior belong.
Another means of understanding the relationships among various forms of disruptive behavior comes from meta-analytic reviews of the literature that have employed factor analysis to study these relationships. One such review by Paul Frick and colleagues (1993) showed how various forms of oppositional behavior may cluster into a form of overt disruptive behavior that is nondestructive but is related to three other equally, if not more serious, forms of antisocial acts, status violations, and aggression toward and offenses against others. As such, childhood oppositional behavior carries significant concurrent and developmental risks for more serious forms of externalizing disorders, such as conduct disorder (CD), and the co-existence of CD with ODD is itself a strong predictor of concurrent and later antisocial or criminal activity and substance use and abuse. Childhood oppositionality also conveys an increase in risk for later anxiety disorders and depression in addition to its known association with CD. The link between ODD and anxiety may be mediated, in part, by the comorbidity of each with ADHD.
Degrees of Oppositionality (Noncompliance-Defiance or ODD)
As
the foregoing discussion makes apparent, there exists a continuum of
oppositionality in the human child population along which degrees of
oppositionality, defiant or noncompliant child behavior, can be discerned. Whereas degrees of intellectual deficits may
be carved into categories of slow, borderline, mild, moderate, and severe or
profound to define mental retardation, no such consensus exists for labeling
degrees of noncompliant or defiant behavior, though adapting some of the former
categories might be appropriate for a dimension of defiant behavior. On a
well-standardized behavior rating scale of this dimension, children whose
defiant behavior exceeds the mean by only one standard deviation (+1 SD,
84th percentile) or less are considered normal even though possibly being
stubborn or strong-willed. Those children placing above the 84th percentile but
below the 93rd percentile (within +1 to +1.5 SD) could be described as
having borderline oppositionality or just as being “noncompliant” or “difficult,” provided they do not meet the full
clinical diagnostic criteria for ODD in the DSM-5. Those children who place
above the 93rd percentile on such rating scales or who meet full clinical
criteria for ODD by diagnostic rules would be said to have that disorder,
perhaps further qualified as mild, moderate, or severe depending on the
severity of their ratings of deviant behavior on the rating scales or the
number of ODD symptoms they possess above the minimal number required to meet
the diagnostic threshold. Children in most of these categories except the
normal one might be appropriate for this parent training program, provided that
the criteria for justifying intervention described above were met.
Prevalence of ODD
As summarized by McMahon and Frick (2019), studies show that the frequency with which children manifest clinically significant and impairing levels of defiant and noncompliant behavior is greatly determined by the definition used for such disorders when surveying childhood populations. The lifetime prevalence rate of ODD appears to be 10.2% but with ranges being reported from 2.6% to 28%, depending of course on how it is defined and assessed. In large scale studies, the prevalence of ODD in children seems to be around 6%. DSM-IV cited a prevalence ranging between 2 and 16% for ODD. Using parent reports of child behavior problems in a large sample (1,096) of military dependents ages 6 to 17-years-old, one study reported a prevalence of 4.9% for ODD based on diagnostic criteria from the DSM-III-R. Another study using multiple sources of information (parent, child, teacher) for a large sample of 11-year-olds reported a prevalence rate of 5.7% for ODD using DSM-III diagnostic criteria. In the child age group, the male-to-female ratio for ODD can range from 2:1 to 3:1 but by adolescence the sex ratio is nearly equal. There is a decrease in the prevalence of ODD with age with up to half of all cases in childhood not meeting criteria for the disorder in later years.
Relationship of ODD to Other Disorders
As noted earlier, childhood ODD is strongly associated with risk for concurrent or eventual childhood CD (see Thapar & Goozen, 2019). Although approximately 20-25% of children with ODD may no longer have the disorder 3 years later, up to 52% will persist in having ODD over this period of time. Of those who persist with ODD, nearly half (25% of the initial total of ODD children) will meet criteria for CD within a 3-year follow-up period. However, among children who have CD, over 80% will have had ODD as a co-existing or even preexisting disorder, making ODD the most common early developmental stage for the co-existence with or later progression into CD. And so, while the majority of ODD children will not progress further into CD, children with persistent ODD are more likely to do so, and the vast majority of children with CD will have ODD. The age of onset of early CD symptoms has been shown repeatedly to be a particularly important predictor of the progression into delinquency and the severity and persistence of such delinquency, with onset of initial symptoms before age 12-years-old being an especially salient threshold in making such predictions.
Beyond its relationship to CD, ODD also carries a high risk for the co-existence or development of other psychiatric disorders, such as ADHD, depression and even anxiety disorders. Nock et al. (2007) found that over 92% of people who have qualified for ODD in their lifetime had at least one other lifetime psychiatric disorder, with risks being 46% for mood disorders, 62% for anxiety disorders, 68% for ADHD or other impulse control disorders, and 47% for substance use disorders.
ADHD shows a strong linkage to ODD; ADHD children are up to 11 times more likely than non-ADHD children to eventually be diagnosed with ODD. ADHD is also linked to the persistence of ODD. ADHD has an earlier average age of onset than ODD with up to 60% or more of children with ADHD eventually developing ODD, often within a few years of the onset of their ADHD. It appears to be the hyperactive-impulsive symptom dimension of ADHD that is most strongly predictive of the eventual development of ODD and especially the head strong, defiant, or social conflict aspects of ODD or oppositionality to be discussed below. In view of the above, it is apparent that early hyperactive-impulsive behavior is a childhood risk factor for the development and persistence of ODD. Yet research has also repeatedly demonstrated that impaired or disrupted parenting along with associated parent psychopathology is among the most influential predictors of which children progress from being ADHD only to developing ODD. The emergence of ODD is then a risk factor for concurrent or later CD, anxiety, and depression. And all three externalizing disorders (ADHD, ODD, and CD) are predictors of later adult criminal behavior and arrest rates.
The Nature of Parent-Child Interactions in Defiant Children
The
substantial body of research that exists on the parent-child relations in
families with oppositional children is too voluminous to review here. At the
very least, interested readers should begin with a perusal of the texts by
Patterson (1982; Patterson et al., 1992) and others (McMahon & Forehand,
2005; Wahler, 1975) for their historical importance and insight into the family
interactions of aggressive or defiant children. The texts by Patterson and
colleagues in particular set forth one of the most well-established and
accepted theories concerning the development and maintenance of oppositionality
and aggression in parent-child interactions, known as coercion theory and discussed further below. Coercion theory falls within the larger
framework of social learning theory which is a major part of if not the
foundation for the development of all behaviorally oriented parent training
programs, including this one. This theory simply
states that noncompliant, defiant and aggressive child behavior arises from
and/or is largely sustained by the family context and especially by the social
consequences such behavior receives from others within the family. Thus, to
the extent that such behavior is being learned and maintained within families,
it can be unlearned, reduced, or returned to a normal state by unlearning, or
through the alteration of the contributing contingencies within families. For
more contemporary reviews on the nature of oppositionality generally and ODD
specifically in children one should read the chapter by Hinshaw and Lee (2012)
as well as published reviews or studies by Beauchaine, Hinshaw, and Pang,
(2010), Burke et al. (2008), Ellis and Nigg (2009), Loeber et al. (2009), Nock
et al., (2007), Rydell (2010), and Harvey et al. (2011). The more consistent
and general findings from this body of research are important for clinicians to
consider when engaging in the training of these families. I summarize them
briefly below.
Without a doubt,
research repeatedly demonstrates that the quality or nature of parent-child
interactions is strongly and reliably associated with childhood noncompliant,
defiant, and aggressive behavior patterns, and the persistence of these behaviors
over development, as well as the risk for later adolescent delinquency and
conduct disorder. Children with oppositional behavior show a poorer quality of
attachment relationships to their parents along with their significantly higher rates of stubbornness,
verbal defiance, temper outbursts, arguments, and even physical aggression in
their interactions with their parents (and other family members). The parents
of such children also provide highly inconsistent, lax, and, at times, even
positive consequences to children for their deviant behavior.
Such poor attachment, unpredictable use of consequences, and even inadvertent
reinforcement of defiant behavior may serve to increase and sustain occurrences
of oppositional child behavior in future interactions. When children fail to
comply with parental directions and rules, and especially when they refuse to
obey, act out, throw temper tantrums, engage in aggression toward parents, or
otherwise directly oppose commands, it is surely difficult for parents not to
attend to such behavior. Even though such attention is largely negative in
nature and involves high rates of expressed hostility and other negative
emotions, it may still serve to sustain or increase future oppositional
behavior. On other occasions, paternal
laxness in discipline may also contribute to child ODD symptoms across
development, perhaps signaling to the child that there will be no consequences
for oppositional behavior toward either parent.
Parents may also provide positive attention or rewards to children in an effort
to get them to stop “making a scene,” such as in a store, restaurant, or other
public place. Buying a child the candy bar or toy for which he has been throwing
a tantrum is but one obvious way in which parents may accelerate the
acquisition and maintenance of oppositional child behavior.
Conversely,
parents may provide less attention or reinforcement to prosocial or appropriate
behaviors of the child. Clinical experience suggests that parents of
oppositional children may monitor or survey child behaviors less often than in
families of normal children, such that they may not always be aware of ongoing
appropriate child behaviors. Even if they are
aware that the child is behaving well, they may elect not to attend to the
child or praise him for several reasons. One is that many parents report that
when they praise or attend to good behavior in their oppositional child it only
serves to provoke a burst of negative behavior from the child. This leads the
parent to adopt the attitude of “let sleeping dogs lie” when they encounter
ongoing acceptable child behavior. Research has not established that this
reaction occurs when parents have tried to praise a behavior problem child or,
if it does, what the learning history was that established this behavioral
pattern. But it is a frequently voiced opinion by parents of these children in
my clinical experience. It is possible that parental praise for good behavior
in a child prompts the child to misbehave because the child continues to
receive parental attention if he/she does so. Had the child continued to behave
well, the parent might have terminated the interaction, moving on to do something
else. Another reason parents may fail to react positively when a defiant child
behaves well is that parents dislike interacting with the oppositional child
and will choose to avoid interacting with the child when possible, reducing
their contact with this temperamental individual. Parents of chronically
defiant children often develop animosity or “grudges” toward the child such
that they will elect not to praise him when the child finally behaves well.
This may eventually lead to parents spending significantly less leisure and
recreational time with the defiant child simply because it is not fun to do so.
In addition, it
is possible that parents of oppositional children, especially those children at
risk for later delinquency, may monitor their children’s activities less often
and attend less to unacceptable behavior so as to avoid
further confrontations with the child. As in the saying “out of sight, out of mind,”
parents may eventually reduce the amount of effort they expend monitoring a
child’s ongoing behavior within the home so as not to have to confront any
minor unacceptable behavior that may be occurring. By overlooking the problem
behavior, they do not have to face the aversive nature of dealing with this
difficult child or otherwise engage in yet another negative, coercive exchange
with the child about the matter. This may explain the frequent clinical
observation that some parents seem to be oblivious to ongoing negative behavior
occurring in their presence – behavior other parents would normally react to in a
corrective fashion. For various reasons to be explored further below, some
parents of oppositional children are simply not as invested in serving in parental
roles to these children, possibly because of their own frequently
younger-than-normal age when becoming parents, single motherhood status, their
social immaturity or limited intelligence, and even their own psychological or
psychiatric disorders. Regardless of its origins, such a decline in parental
monitoring and management of a child’s activities generally is associated with
the development of some of the most serious forms of CD, which involve both
covert antisocial behavior – such as lying, stealing, destruction of community
property, and so forth – as well as overt antisocial acts, such as physical
aggression toward others.
Parents may also
be observed actually to punish prosocial or appropriate behavior at times,
again because of possible resentment that may have developed over years of
negative interactions with the child. Parents may often give “back-handed
compliments” to a child for finally doing something correctly, as when they
sarcastically remark, “It’s about time you cleaned your room; why couldn’t you
do that yesterday?” For all of these reasons, parents are simply not providing
appropriate, consistent, or even contingent consequences for ongoing child
behavior that would be expected to manage or control it effectively.
This
inconsistent, over-reactive, sometimes timid or lax, and often unpredictable
use of consequences is a hallmark of parents who have highly oppositional
children. It is characterized by both punishing both prosocial and antisocial
child behavior as well as intermittently and unpredictably rewarding both
classes of child behavior. Termed “indiscriminant”
parenting, the oppositional children in these interactions are damned if they
do and damned if they don’t comply. Dumas and Wahler (1985) have hypothesized
that this form of indiscriminant use of consequences by parents creates a great
deal of social unpredictability within families and especially in the
parent-child relationship. Such environments are experienced by both humans and
animals as inherently aversive. Any response by the child in such a situation
that may be instrumental in reducing unpredictability (increasing
predictability) will be negatively reinforced for doing so and thereby increase
in frequency. Thus, according to this theory, children may emit various forms
of defiant and aggressive behavior toward parents, based on which of these
forms increases predictability in the course of parent-child interactions.
Even more evidence exists for the role of negative reinforcement in these interactions, as explained in the highly influential coercion theory developed by Patterson (1976, 1982) and colleagues. This research group has argued that both parents and children in families with defiant or aggressive children are negatively reinforced for behaving in aggressive and coercive ways toward each other, and that such negative reinforcement serves to sustain their highly conflicted and hostile interactions with each other. Substantial research supports this argument.
To understand
this theory, it is first necessary to remember that negative reinforcement is not the same as punishment – a mistake often made by those less experienced in behavioral
terminology. Negative reinforcement occurs when a particular behavior serves to
reduce or terminate an unwanted or aversive interaction or situation. This
reduction in unpleasantness or in the aversive nature of the situation is
reinforcing and serves to increase the probability that the person will employ
that same behavior in the next encounter with that or a related aversive
situation.
In this theory,
the negative or aversive behavior of one member of the parent-child dyad serves
to terminate the ongoing negative behavior of the other, thereby negatively
reinforcing the first member’s “coercive” behavior. The use of angry, hostile,
defiant, or aggressive behavior by one party serves to coerce the other party
to reduce or terminate the conflicted interaction, hence the term coercion
theory. Important to appreciate here is that both parties are using such
coercive tactics with each other (though not necessarily intentionally) and so
both are subject to the operation of negative reinforcement that serves to
sustain this reciprocal chain of negative interactions. On some occasions one
person’s coercion succeeds in the withdrawal of the other from the interaction
or at least in a reduction in the aversive nature of the interaction. Yet on
other occasions the other person’s negative behavior succeeds, and so both
participants are involved in a partial reinforcement schedule. Such schedules
are known to generate some of the most persistent behavior, in this case of
negative or hostile conduct thereby explaining the persistence of such
conflict-ridden family interactions. Over time, each party learns that it takes
an ever higher level of hostility, aggression, or generally aversive behavior
to cause the other party to reduce or terminate the interaction. This
presumably explains why parents and children, once having begun a negative
interaction with each other, will escalate their negative behavior toward each
other very quickly to intense levels of anger, hostility, aggression or general
coercion. Furthermore, the likelihood that such forms of interaction will occur
again is greatly increased as a result.
As an example,
consider what may ensue when the parent of an oppositional child attempts to
impose the command of getting ready for bed while the child is watching a
favorite television program. Like many children, this child often finds this
imposition to be aversive, unpleasant, or otherwise unwanted. The child may
oppose, resist, or otherwise escape from the parental demand through defiant,
aggressive, or other coercive behavior. The parent withdraws from the
interaction, at least temporarily, and so that behavior by the child may serve
to delay having to get ready for bed and allows the child to continue to remain
up and watching television. The child’s success at escaping from the command,
even if only temporarily, negatively reinforces his/her oppositional behavior.
The next time the parent asks the child to get ready for bed, the likelihood of
the child resisting the command has increased. The more a parent persists at
repeating the request, the more intense the child’s resistance may become due
to this previous success at escaping or avoiding the activity specified in the
command. As already noted above, many parents may eventually acquiesce to this
type of coercive child behavior. Parents need not acquiesce to every command
for a child to acquire resistant behavior; only to some of them.
Parents may also
acquire aggressive or coercive behavior toward their defiant child by much the
same process. In this case, the parent may have been successful on occasion at
getting a child to cease whining, refusing, or throwing a tantrum and to comply
with a command through the parent’s use of yelling, screaming, or even physical
aggression against the child. The parent may also have discovered that rapidly
increasing the intensity of his/her negative behavior toward the child is more
successful at getting the child to capitulate and obey, especially if the child
initially opposes the command. Hence, in subsequent situations the parent may
escalate very quickly to intense yelling, use of threats, and other negative
behavior toward a child due to a previous history of its success at terminating
oppositional child behavior by this means. The parent need not be successful
with this strategy every time or even the majority of times the parent
confronts oppositional behavior in order to maintain this type of parental hostile
behavior across most command-compliance encounters with the defiant child. Only
occasional success with coercive behavior is needed to sustain this type of
behavior in parents.
Viewed from this
perspective, both parent and child have a prior history of periodic but only
partial success at escaping or avoiding each other’s escalating aversive or
coercive behavior. Each can be considered both the victim and the architect of
this coercive family process. As a result, each will
continue to employ it with the other in most command-compliance interactions.
Over time, each learns that when a command-compliance situation arises, the
faster each escalates his/her own negative emotional intensity and
coerciveness, the more likely the other is to acquiesce to his/her demands. As
a result, over months of experience with each other, confrontational
interactions between parent and child may escalate quickly to quite intense,
emotional, and even aggressive confrontations. On some occasions these may end
with physical abuse of the child by the parent, destruction of property by the
child, assault by the child against the parent, or even self-injury by some
children.
This view also
implies that much oppositional child behavior is not sustained by positive
attention or reinforcement from the parent but by negative reinforcement. Accordingly, when a clinician
tells such a parent to ignore negative child behavior, it may only worsen the
problem as it is likely to be viewed by the child as acquiescence. In many
cases, parents cannot ignore the child because in so doing the child escapes
from performing the command given by the parent. Parents in such a situation
will have to continue interacting with the child if they wish to get the task
accomplished. Many experienced clinicians have noted this problem in training
parents of behavior problem children – ignoring defiant behavior is not always
successful or even possible. Instead, a great deal of negative child behavior
is developed, not through positive parental attention, but through
escape/avoidance learning (negative reinforcement). It is maintained because of
its success in avoiding unpleasant or aversive activities often invoked by
parents. As Patterson suggests, and as this program teaches, the parent
training program must incorporate mild and consistent punishment
(usually time out from reinforcement), as well as prevention of the child from
escaping the parental command, if the program is to be successful at diminishing
child noncompliance developed through such a process of negative reinforcement.
Patterson has
also noted that parents are likely, once trained, to rely
predominantly on the punishment methods taught in the program and to diminish
their use of positive reinforcement methods over time. Therapists must
anticipate this parental drift and regression and address it during the last
few sessions of parent training as well as during follow-up booster sessions.
Parents must be instructed that most punishment methods lose their
effectiveness when relied on as the primary management technique with children.
Without sufficient positive reinforcement methods being provided for the
alternative, appropriate behavior desired from the child, such desirable behavior
is unlikely to be maintained.
Understanding the Multivariate Causes of Oppositionality and Defiance in
Children: The Four Factor Model of Child Oppositional Behavior
The factors that
contribute to oppositionality can be nicely summarized in a model comprising
four factors. Each of these factors will now be discussed in some detail.
Factor I: Coercive Family Processes Operating in the Parent-Child
Relationship
As discussed
above, and shown in Figure 1, below, one of the major if not greatest proximal contributors to noncompliance,
defiance, and social aggression repeatedly identified in research studies is
disrupted parenting. By this is meant ineffective, inconsistent,
indiscriminant and lax or even timid child management methods being employed by
parents, often but not always combined with high rates of expressed hostile
emotions and at times including unusually harsh (abusive) but inconsistent
disciplinary methods. In the case of ODD children who develop CD as well, one also
finds low parental warmth and poor parental monitoring of the child activities
both in and especially outside the home. As a result of even partial success
and employing emotional coercion, noncompliance and defiance by children become
very effective methods for escaping or avoiding unpleasant, boring, or
effortful tasks. This partial success of mutual, reciprocal coercion is more
than enough to sustain the persistent use of aversive, hostile, and aggressive
behavior by each party toward the other. The child’s use of coercion may also
serve to increase the predictability of consequences in parent-child exchanges
(no matter how negative), and on some occasions even obtaining rewards by the child
for doing so (e.g., candy for the tantrum in the store). Thus, mutual coercion
is a major pathway through which oppositionality in children and heightened
parent-child conflict can arise. But it would be erroneous to conclude from
this that all defiant behavior is simply learned out of the parent-child
relationship. Social learning theory can only get us so far in understanding
the development and evolution of oppositionality and social aggression in
children (or their parents).
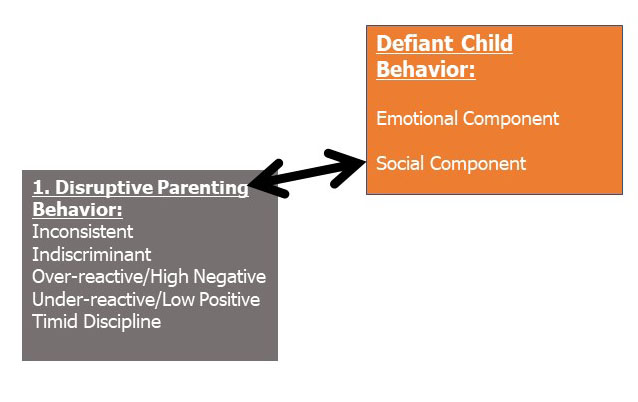
Figure 1
Whereas the exact form, nature, or topography of
the noncompliant and defiant responses and even their severity in a child
probably have much to do with the child’s learning history within a family, the
probability of acquiring or emitting oppositional or noncompliant behavior and
some of its severity is also affected by at least three other domains of
influence. Combined with disrupted child and family management practices (first
factor), these three other causal influences make up a Four-Factor Model of
oppositional behavior in children.
Factor II: Predisposing Child Characteristics
Are some
children more likely than others to initiate disruptive, oppositional, or
noncompliant behavior more than others? Unequivocally, yes. The second factor
in the model acknowledges this fact. It is founded on abundant evidence that
children having certain temperaments, psychological traits, and other personal
characteristics are far more prone to emit coercive-aggressive behavior and
acquire defiant or oppositional conduct than are other children.
Research has
demonstrated that child oppositionality consists of at least a two or even
three factor structure each of which can, themselves, be traced back in
development to at least two earlier predisposing characteristics of the child.
Let us start with the two factor structure of oppositionality. Contrary to its representation in the
DSM-IV and even on some child behavior rating scales, oppositionality in
children (or ODD) is not a unitary dimension of symptoms but constitutes two
(or even three) distinct yet inter-related dimensions worth differentiating.
The first of these is an emotional dimension consisting of impatience, irritability, quickness to frustrate or be annoyed, anger, and hostility. It may also include a reduced fear of and diminished sensitivity to punishment, though these seem more likely to be an aspect of childhood psychopathy than of this dimension of ODD. This factor is shown in Figure 2, below.
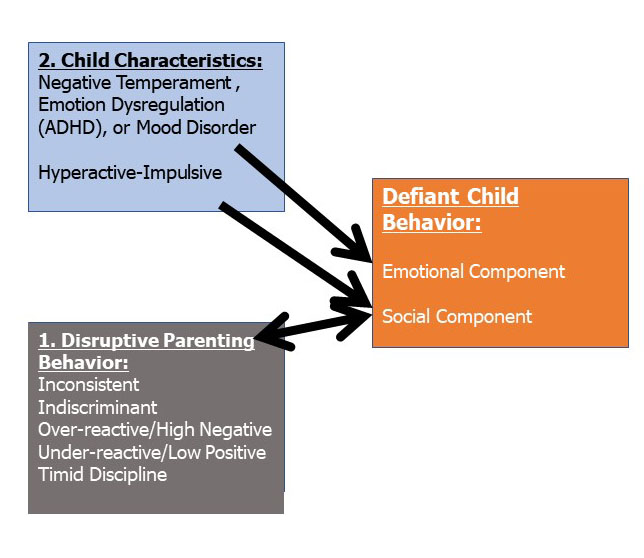
Figure 2
Part of oppositionality is a mood disturbance and that mood is irritability or quickness to anger. It is largely an inherent characteristic of the child and can be traced back into early childhood by its connection to negative or irritable child temperament. Negative child temperament has been repeatedly linked to childhood oppositionality. And although parental psychopathology and poor marital and family functioning may further exacerbate the risks of such children for greater defiance and aggression, negative temperamental features of the child are among the strongest influences in this process and may be sufficient in themselves to create these risks. The effects of early childhood temperament may be gender specific: More negative temperament in infant and toddler boys may be predictive of higher risk for later oppositional behavior; in contrast, for toddler girls early negative temperament may predict a decrease in the risk for later aggressive behavior but possibly an increase in later risk for internalizing disorders.
Whether or not
it arises from a further developmental blossoming of an inherent negative
irritable infant/child temperament in particular cases, this emotional
dimension of ODD can also arise from the presence of a psychiatric disorder in
the child that disrupts normal emotion regulation. The two, in fact, often
co-exist (irritable temperament and early emotional dysregulation). Disorders
such as childhood onset bipolar disorder, depression, and ADHD, among others,
are all predisposing factors to the development of comorbid ODD and the pathway
for doing so is in part their impact on emotion regulation.
For instance, ADHD is known to be associated with impulsive emotions and deficits in executive functioning one dimension of which is emotional self-regulation. It is therefore associated with significantly higher rates of impatience, verbal aggression, and anger than is typical of the childhood population. Indeed, ADHD shares this dimension of heightened emotionality with ODD specifically and the dimension of externalizing psychopathology in children more generally; a shared risk arising both from shared genetic liability and an environmental liability, such as Factor I above. Disorders like ADHD or mood disorders that create increased emotion, emotional dysregulation, or the impulsive expression and deficient (executive) self-regulation of emotion thereby create a propensity toward ODD through its first or emotional dimension – irritability, impatience, and quickness to anger.
Going forward in development, this emotional dimension is significantly associated with risk for depression specifically, mood disorders more generally, and even anxiety disorders by adolescence, if not earlier. It may also increase the risk for symptoms of autistic spectrum disorders and even schizophrenia symptoms. This risk for mood and thought disorders appears to be the case in both sexes of children, though especially in girls.
The second dimension of ODD is one of defiant behavior or social conflict or a propensity to be head strong. A propensity for rule-breaking, stubbornness, noncompliance or a direct refusal to obey, ignoring the requests of others, such as parents, high rates of exploratory activity (hyperactivity), impulsive, excessive, and even defiant verbal behavior, and physical resistance to the demands of another all comprise this second social conflict or head strong dimension. This dimension of ODD or oppositionality is related to an earlier childhood history of persistent hyperactive-impulsive (HI) behavior more than it is to earlier inattentive symptoms. This explains why high temperamental activity or ADHD (hyperactive or combined types), again, is often a major precursor to ODD through its contribution to the head strong or social conflict dimension of ODD. It should be evident here that pre-existing ADHD or its early infant/child temperament precursors can contribute to ODD through both of its dimensions. The impulsive emotion and poor self-regulation of emotions associated with ADHD can contribute to the emotional dimension of ODD while the HI dimension of ADHD symptoms (that includes the impulsive expression of emotions) can also contribute to the head strong dimension of ADHD and thus its propensity to cause social conflicts with others, initially parents. It is not surprising then that there exists a single shared genetic liability to both the HI dimension of ADHD and to this head strong dimension of ODD and between these two factors and concurrent and later conduct problems or disorder. This may explain why ODD is 11 times more likely to occur in the context of ADHD than in the general population given that ADHD is a contributor to both ODD dimensions and accounts for any genetic (heritable) liability to ODD and even to later CD.
Symptoms of ADHD, such as over-activity, inattention, and impulsivity, are typically considered aspects of early childhood temperament when studied in infants and toddlers, believed to be a harbinger of later personality traits. Should these temperamental traits persist into later preschool years and eventually school age, such symptoms are more likely to create persistent parent-child interaction conflicts and parenting stress. Symptoms of ADHD may prevent a child from finishing assigned activities or otherwise adversely affect their interactions with parents and thus the child may be more likely to elicit increased commands, supervision, and negative reactions from parents. The relationship here may be reciprocal, with the child’s poor attentional control adversely affecting parental responses which may then reciprocally adversely affect the child’s further development of attentional control. Children with higher levels of ADHD symptoms may also be more likely to respond to parental controlling behavior with impulsive negative emotional reactions. If such reactions result in the child’s escaping further demands, according to the above coercion theory of defiance, their use during subsequent commands by parents will be increased and sustained. The co-occurrence of ADHD symptoms, particularly that of poor impulse control, with early oppositionality is particularly virulent, predicting significantly greater family conflicts and worse developmental outcomes, especially in the realm of later antisocial activity, than does either dimension of behavior alone.
Though early HI
behavior is a clear contributor to this behavioral dimension of ODD, as just
noted social training via earlier and concurrent inconsistent parenting is
likely to operate through this dimension of ODD as well. Indeed, it may
mediate the relationship of HI symptoms to ODD in that a context of disruptive
family routines or inconsistent parenting may determine if HI will increase the
risk for ODD. The excessive behavior of the highly
HI child results in a greater frequency of rule violations and also brings them
into repeated conflict with those trying to manage, supervise, and otherwise
rear them. The heightened emotionality of the child further ensures that they
will respond to efforts of parental control with a greater propensity for
irritability, anger, and hostility. Whether this progresses further to clinical
ODD may well depend on the parental response to it and the consistency and
predictability of family routines. If this barrage of high rate behavior and
emotionality by the child is responded to by inconsistent or over-reactive
parenting, high levels of parental expressed emotion, parental timidity in
using effective discipline, disrupted or unpredictable family routines, and
parental child-rearing disagreements, the training ground for further
oppositionality and defiance via the coercive family process described above
has now been set in motion.
This involvement of parenting in this dimension of ODD also helps to understand why studies often find that there is a situation specific factor or context to ODD besides its emotional and behavioral/social dimensions. That is to say that ODD can be highly situation and person specific and is most often seen in parent-child interactions. While it can be seen as well in child-peer interactions or child-teacher interactions, the child and family correlates of children engaging in such peer or even teacher conflicts may not be the same as for those seen in parent-targeted ODD. This situation specificity of ODD, however, may simply reflect the stepping stone model first described by Patterson (1982) in which ODD often first appears in the home toward parents but then may, over time, increases in frequency and intensity and spreads to interactions with siblings. From there, it then metastasizes onward or outward to interactions with other children in the neighborhood or school and eventually even to teachers. In sum, there are both child temperamental or psychological as well as parenting/family environmental contributors to child oppositionality or ODD.
The aforementioned role of disrupted parenting in ODD sheds light on understanding why ODD is also just as familial a disorder as ADHD. That is to say that families in which ODD exists in their children are far more likely to have other family members who meet criteria for ODD than families having no psychopathology. ODD can be a family diagnosis and not just a diagnosis of the child member of that family. This would be expected from the high heritability of ADHD traits such as HI and impulsive emotional symptoms and their shared genetic liability with ODD making these traits more likely to be evident in biological relatives as well as from the reciprocal coercive family training taking place across repeated parent-child interactions.
This seems to make it clearer now how this behavioral dimension of ODD is more predictive over development of concurrent and later risk for CD in both males and females, although the emotional dimension of ODD may convey some risk for CD as well. It is the dimension most associated with rule-breaking, defiance of authority, and conflict with others more generally. It also makes it apparent why early HI symptoms may increase the risk for CD indirectly via their contribution to this head strong behavioral dimension of ODD and from there on to CD.
A third smaller dimension of ODD has sometimes been identified by researchers, though not consistently, and typically referred to as hurtful. It consists of the physically aggressive and vindictive symptoms that can co-exist with ODD or child oppositionality. But this dimension of physical aggression may actually be more of a feature of early CD than of ODD. Verbal aggression is more highly associated with ODD while physical aggression is more strongly linked to CD. Even so, early verbal aggression is a significant predictor of the later development of physical aggression accounting for why ODD increases the risk for later CD. It therefore seems best to view any hurtful or physically aggressive dimension of behavior as reflecting CD rather than ODD.
While not
considered to be a dimension of ODD, another component of child psychological
development related to this broader class of externalizing psychopathology
(ADHD, ODD, CD) is important to at least briefly note here given its higher than
normal occurrence in some children with ODD and especially some cases of CD.
That dimension is the callous-unemotional (CU) traits evident in childhood
psychopathy. There is strong evidence for the role of genetics and neurology
in the development of CU traits or psychopathy in comparison to a much weaker
role for social causes. Such children demonstrate a
significant lack of empathy for the misfortunes of others and a lack of guilt,
conscience, and remorse for their own transgressions. They may also show a
reduced insensitivity to and fear of punishment. Indeed these latter
attributes may not be so much a part of the emotional dimension of ODD as first
noted above but rather a signal for the presence of these CU traits in such a
child. This CU dimension is known to be associated with or predictive of
concurrent, more severe and more persistent forms of antisocial behavior in
children and adolescents and of risk for antisocial personality disorder in
adults even independently of ODD and CD.
To summarize,
ODD appears to consist of two separable yet inter-related psychological
dimensions. One is comprised of an emotional dimension that may emerge in part
from early childhood negative/irritable temperament as well as from the early
emergence of symptoms of mood disorders. It is associated with an elevated
risk for later mood and anxiety disorders by adolescence if not earlier. The
other is a behavioral dimension comprised of defiance, rule breaking, verbal
aggression, and otherwise head strong behavior that emerges from or is related
to earlier persistent hyperactive-impulsive behavior interacting with coercive
family processes that provide reciprocal negative and partial reinforcement to
both parent and child for angry, hostile, stubborn, and verbally aggressive
interactions. It is associated with an elevated risk of current or later CD.
These two dimensions are sometimes joined by a third one comprised of hurtful,
vindictive, or otherwise physically aggressive behavior that, while not an
inherent part of ODD, can co-exist with it and is more highly related to
concurrent or later CD. A fourth dimension may also be apparent in some
children that consists of CU traits comprising childhood psychopathy and
predictive of even more persistent antisocial behavior and adult antisocial
personality disorder.
Factor III: Predisposing Parent Characteristics
As in the case
of child characteristics above, are some parents more likely than others to
engage in coercive parenting practices and to have more defiant children?
Again, undoubtedly yes. Noncompliance or oppositionality in children may also
increase in probability in children as a result of this third factor; that is,
predisposing parental characteristics. For instance, the risk of child
disruptive behavior is elevated in families as a function of the earlier age of
mothers at the time of child-bearing, and this effect is greatest on second and
third born children. This factor is illustrated in Figure 3, below.
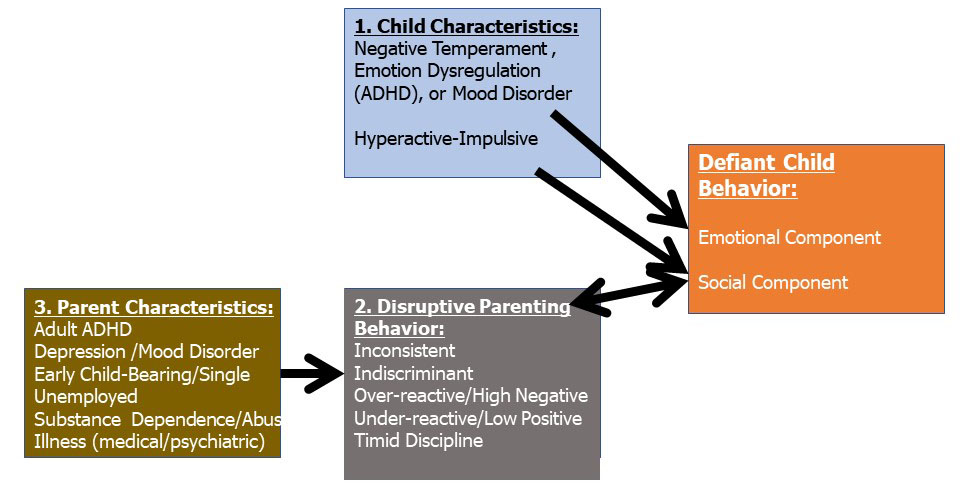
Figure 3
ODD children, especially those with comorbid ADHD, are also more likely to have parents with psychiatric disorders, especially ADHD, depression, and antisocial personality disorder, than are children without these disorders. Conversely, immature, inexperienced, impulsive, inattentive, depressed, hostile, rejecting, or otherwise negatively temperamental parents are also more likely to have defiant and aggressive children. It is certainly likely that some of the risk of shared parent and child psychiatric disorders, as in ADHD and depression, and even parent-child hostility is a consequence of shared psychiatric genetics and not because the parental disorder conveys an environmental (parenting) risk for the child’s disorder, such as ODD. Yet research shows that parental disorders like depression and ADHD convey a risk as an environmental liability (disrupted parenting) for the child independent of the risk conveyed genetically for the child’s disorder.
This is because
ADHD, depressed, antisocial or otherwise psychiatrically impaired parents
display poor attention and monitoring abilities around their children,
inconsistent management strategies, greater use of negative parenting methods,
and higher levels of irritability, hostility, and expressed negative emotions
toward their children, and provide less positive parenting methods and
reinforcement for prosocial behavior. Through
such inconsistent, over-reactive, and indiscriminant parenting, then, parents
set in motion a reciprocal coercive family process in which children experience
periodic success at avoiding demands, further reinforcing the children’s use of
oppositional or coercive behavior. Such increases in child coercive behavior
may then feed back further to affect detrimentally parent mood, sense of
competence, self-esteem, and even marital functioning in a vicious, reciprocal
cycle of bidirectional effects. Such parents may also employ coercive behavior
with others in the family, providing a model of such behavior for the child to
imitate.
Parents of children with externalizing disorders, like ODD, are more likely to have problems empathizing with their child, to have an inappropriate or external locus of control, to demonstrate low frustration tolerance, among other cognitive and attributional disturbances or biases, and to show disrupted synchrony in their parent-child interactions. These cognitive risk factors appear to make their own contribution to the evolution of child behavioral problems independent of their impact on disrupted parenting. Some of these cognitive risk factors are also highly related to likelihood of parental aggression toward their children, accounting for 63% of the variance in parental abuse potential and 55% of the variance in parental inappropriate disciplinary practices.
Where parents have a specific psychiatric disorder, it may further adversely impact parenting. More specifically, the level of parental ADHD, parental depression, and parental antisocial personality disorder, are significantly associated with risk for parenting stress and disrupted parenting. As a consequence, these parental disorders pose an increased risk for their children developing oppositional and aggressive behavior and later CD or delinquency.
The presence of these disorders, particularly parental ADHD, is also a predictor for reduced success or even failure in behavioral parent training programs such as this one. For these reasons and those noted below for contextual factors, parent psychological status must be a formal focus of the evaluation of children referred for defiant behavior. Indeed, parental ADHD or depression may require treatment before involving such parents in training in order to improve their pre-treatment parenting abilities, such as with stimulant medication in the case of adult ADHD, and thus increase parents susceptibility to successful training.
Factor IV: Predisposing Contextual Factors
It is virtually
self-evident that parental behavior is not only a function of various parent
characteristics or attributes that may predispose parents toward using
disrupted parenting methods but that parental behavior may also be adversely
affected by the surrounding social ecology or family context. A few factors
acting within this context have been identified, and this context serves as the
fourth factor in the model shown in Figure 4, below.
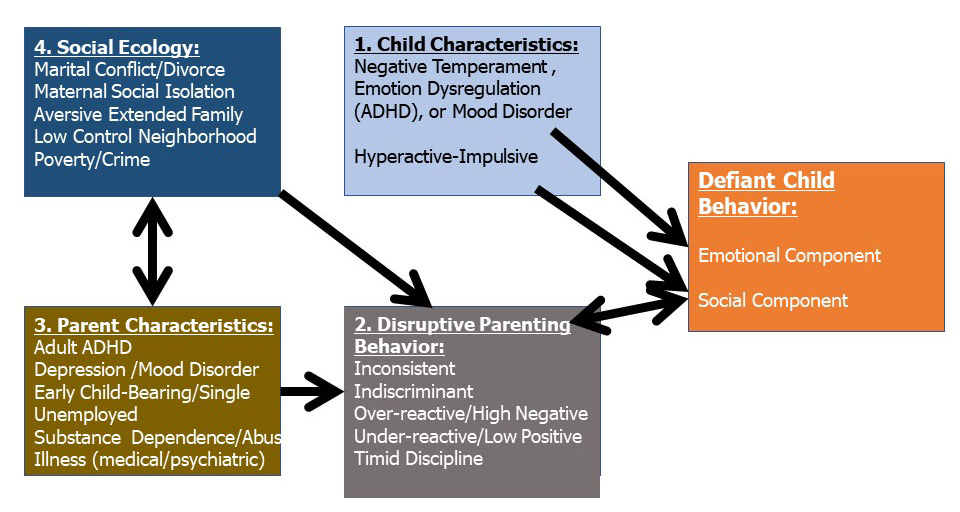
Figure 4
Certain characteristics of the
family context may create or contribute to increased risks for child defiant
behavior and aggression as well as later delinquency. As
noted earlier, maternal social isolation is one such factor. But
so is parental marital status. Single mothers are the most likely to have
significantly aggressive children, followed by mothers who live with male
partners but are unmarried. Married mothers have the lowest
rates of aggressive children, with these associations being moderated somewhat
by higher socio-economic status.
Marital discord also has been repeatedly linked to child disruptive and defiant behavior, especially high intensity couple conflict. Apart from marital discord, parental disagreement over child-rearing may make independent contributions to risk for child disruptive behavior. Debate continues over the mechanisms involved in this relationship between inter-parental relations and child disruptive behavior. It may be reciprocal, with marital discord contributing to higher rates of oppositionality in children through its adverse effects on parenting and child oppositionality then feedbacks to worsen marital discord and child-rearing disagreements all of which may hasten divorce.
Also noted
earlier, family social disadvantage or social adversity is another factor
associated with risks for childhood defiant and aggressive behavior. These stress events or settings appear to act on child
misbehavior via their influence on creating inconsistent or indiscriminant
parenting practices, inattention, lower rates of positive parenting, and
parental irritability or aggression in child management by parents. Such
disrupted parental behavior further predisposes children to develop or sustain
noncompliance or defiance within family interactions as noted above.
Notice
that for some of these circumstances, a reciprocal relationship exists wherein
they may contribute to antisocial behavior in a child but such behavior, once
developed, contributes to a worsening of these circumstances, such as in marital
conflict, divorce, and parent psychiatric disturbances. Research with ADHD
children suggests that disruptive and oppositional behavior may also feed back
to increase parental alcohol use as well. I illustrate these feedback mechanisms with additional arrows (effects) in the final Figure 5 of the four-factor model, below.
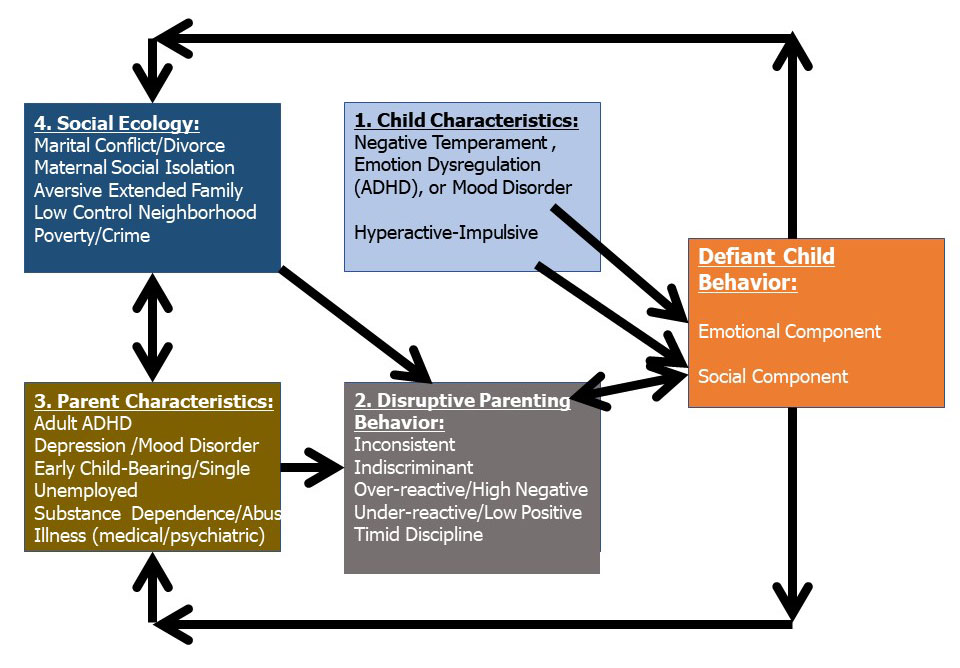
Figure 5. The
four factor model of child oppositional defiant behavior. From R. A. Barkley
(2013). Defiant Children: A Clinician’s Manual for Assessment and Parent
Training (3rd ed.). New York: Guilford Press. Copyright 2013 by the Guilford Press. Reprinted with permission
It is all too
common for clinicians to observe that many families referred for treatment of a
defiant child have most or all of these predisposing characteristics:
temperamental, impulsive, overactive, and inattentive children being raised by
immature, temperamental, and impulsive parents within a family experiencing
greater marital, financial, health, and personal distress in its members, where
management of the child is characterized by inconsistent, harsh,
indiscriminant, and coercive parenting often along with reduced parental monitoring
of the child’s activities.
Given all of this it is not surprising to discover that interpersonal trauma may be a consequence of ODD severity and may also feedback to exacerbate such symptoms while non-interpersonal trauma might actually precede the development of ODD or at least further exacerbate its severity (Mikolajewski & Sheeringa, 2022). Hence, family violence may be both a background factor preceding the development of ODD but especially an outcome of the irritable emotion regulation component of ODD coupled with parental insularity or alienation (Chen et al., 2020).
Rationale for Treating Noncompliance/Defiance
Hopefully
this explication of the four-factor model of defiant behavior shows why any
parent training program cannot simply focus on child noncompliance, defiance,
or ODD. Instead, it must target those social processes in the family believed
to have helped, at least partially, to develop or sustain the child’s
oppositional behavior. These processes were more thoroughly explained above in
the section on the “The Nature of Parent-Child Interactions in Defiant
Children.” Noncompliance or oppositionality is the most obvious product of
these social processes, although there are other significant correlates and
outcomes of these processes, such as comorbidity for other disorders in the
child, maternal depression, parental stress and low self-esteem, lack of a
sense of parental competence, marital discord and divorce, and even sibling
hostility and resentment, to name but a few.
There are many well-established reasons for choosing noncompliance or
oppositionality, and its underlying family processes, as the focus of
intervention.
High Proportion of Clinic Referrals
First, noncompliance, or defiance, in various forms appears to be the most frequent complaint of families referring children to child mental health centers, especially for boys. Over half of all referrals to such clinics are for oppositional or aggressive behavior and this figure rises to more than 74% if symptoms of ADHD are included in the analysis. Although these children may receive various diagnoses of ODD, CD, ADHD, Adjustment Reactions, and so forth, a major concern of the parents or teachers referring such a child is his/her inability to comply with directions, commands, rules, or codes of social conduct appropriate to the child’s age group. Parents may complain that the child fails to listen, throws temper tantrums, is aggressive or destructive, is verbally oppositional or resistant to authority, fails to do homework, does not adequately perform chores, cannot play appropriately with neighborhood children, lies or steals frequently, or engages in other forms of inappropriate behavior. However, all of these behaviors are violations of commands, directions, or rules that were either previously stated to the child or are directly stated in the particular situation. Hence, noncompliance, broadly defined, encompasses the majority of acting-out, externalizing, or conduct problem forms of behavior.
High Levels of Family Conflict
Second, noncompliance underlies the majority of negative interactions between family members and the referred child. Research has shown that disruptive or aggressive behavior from children occurs neither continuously nor randomly throughout the day but instead appears in “bursts” or “chunks.” These are high-rate, often intense episodes of oppositional or coercive behaviors by the child that punctuate an otherwise normal stream of behavior. Research early on suggested that one of the most common precipitants of child noncompliance or defiance is parental or teacher commands or requests.
Such negative
encounters between adult and child seem to take a certain predictable form. The
sequence is initiated by the command given by a parent, typically to have the
child engage in a task that is not considered enjoyable or reinforcing by the
child, such as to have the child pick up his/her toys, clean up his/her room,
or perform school homework. On rare occasions, the behavior disordered child
may obey this first request. This usually occurs where the command involves
some very brief amount of effort or work from the child (e.g., “Please hand me
a Kleenex.”) or involves an activity generally pleasurable to the child or that
may promise immediate reinforcement for compliance (e.g., “Get in the car so we
can go get some ice cream”). In these instances, child probably complies with
the request and the family proceeds into other interactions. This may not seem
especially important but what is actually significant here is the fact that
rarely is such compliance followed by social reinforcement, such as a positive
reaction from the parent that acknowledges appreciation for the compliance.
When such compliance goes unnoted by parents, it frequently declines in
occurrence over time and may eventually only occur where the activity requested
of the child involves something highly intrinsically rewarding and immediately
available to the child. In such cases the child obeys not because of being
previously reinforced by the parent for doing so but because the specific
activity required of the child is itself highly reinforcing. However, it is
often only in a minority of instances that behavior disordered children will
comply with the first commands or requests of parents.
More often, the
pattern of events is that the child has failed to comply with the initial
command, which is often followed by the parent simply repeating the command to
the child. This is rarely met with compliance from the child and so the command
may be repeated again, over and over perhaps as many as 5 to 15 times (or
more!) in various forms yet without the child complying with any of them. At
some point, parental frustration arises and the emotional intensity of the
interaction heightens. The parent may then issue a warning or threat to the
child that if compliance does not occur, something unpleasant or punitive will
follow. Yet, the child often fails to comply with the threat, in part, perhaps,
because the parents frequently repeat it. In so doing, the threats lack
credibility and often go unenforced as well. Over time, both parent and child
escalate in their level of emotional behavior toward each other, with voices
rising in volume and intensity, as well as collateral behavioral displays of
anger, defiance, or destructiveness being shown. Ultimately, the interaction
sequence ends in one of several ways. Less frequently, the parent disciplines
the child, perhaps by sending the child to his/her room, removing a favored
privilege from the child, or even hitting the child. Such discipline often
fails because it is inconsistently applied and is delayed well past the point
where compliance was initially requested. More often, the parent acquiesces and
the command is left uncompleted or only partially completed by the child. Even
if the task is eventually done, however, the child has succeeded in at least
delaying its completion, allowing greater time for play or some other desired activity.
This latter
circumstance (eventual child compliance) may prove quite an enigma to parents
and therapists alike. That is, parents may believe that they have actually
“won,” or succeeded in getting the child to listen, yet they are surprised to
find that the child will again attempt to avoid or defy that same command when
issued again later. Parents may question the therapist as to why the child
continues to misbehave or defy them when he ultimately will be forced to
perform the task. The key to understanding this situation, however, is to see
it from a child’s point of view rather than an adult’s. Adults tend to look at
this situation in its entirety and are able to see that ultimately they will
always make the child perform this command (e.g., “Get ready for bed”). Most
children, however, will not show this breadth of awareness of the entire
interaction sequence, but instead will simply view it as a moment-to-moment
interaction with their parents in which their immediate goal is to escape or
avoid doing the requested task, even if only for the moment. As a result, every
minute the child is able to procrastinate is an additional minute they may
continue to do what they were doing prior to the imposition of the command – an
activity often more reinforcing to the child than what the parents may wish
him/her to do. It is also an additional minute of avoiding the often unpleasant
task requested by the parent; avoidance of unpleasant or aversive activities
is itself a (negative) reinforcer for behavior.
This may help to
explain why parents are often puzzled that the child spends more time avoiding
the requested task, as well as arguing or defying the parents, than it would
have taken to do it. The moment-by-moment procrastination of the child is
doubly reinforcing in this sense, serving to permit continued participation in
a desired activity (positive reinforcement) while, for the moment, successfully
avoiding the unpleasant task being imposed by the parent (negative
reinforcement). The ultimate outcome of the interaction (eventual punishment or
forced compliance) is sufficiently delayed so as to have little, if any,
influence on the child’s immediate behavior.
Acquiescence
occurs when the child fails to accomplish the requested activity. In some
instances, the child leaves the situation. He/she may run out of the room or
yard without accomplishing the task. Or the parent may storm out of the room in
anger or frustration, leaving the child to return to his/her previous
activities. In some cases, a parent may in fact complete the command
him/herself, as is seen when a parent picks up the toys for the child. Or the
parent may assist the child with the task after directing the child to do it
alone. In a few instances, the child may not only succeed in escaping from
doing the task, but also receive some positive consequence as well. This can be
seen in cases where, for example, a mother directs a child to pick up toys, the
child refuses, throws him/herself to the floor, and begins hitting his/her head
against the floor. The mother may respond to this behavioral display out of
fear that the child may injure him/herself, by picking the child up and holding
him/her in her lap while trying to soothe the child’s feelings. As a result,
the child’s tantrum and self-injurious behavior are not only negatively
reinforced by escaping from the unpleasant task initially requested by the
mother, but also are positively reinforced by the soothing attention. It is
likely that such dual consequences for oppositional behavior rapidly accelerate
children’s acquisition and maintenance of such behavior patterns in future
similar circumstances. These acquiescent interaction
patterns can be found to underlie many of the negative encounters between
parents and defiant or noncompliant children. They must be the focus of
treatment if the complaints of the family are to be successfully ameliorated.
Situational Pervasiveness
A third
rationale for selecting noncompliance as the target of intervention is its
relatively greater pervasiveness across settings compared to other behavioral
problems seen in children. Research suggests that children who display
noncompliance or coercive behavior in one situation are highly likely to employ
it eventually elsewhere, with other commands or instructions, and with other
adults or children. Improving child compliance may therefore have more
widespread effects across many situations and individuals than would be seen
had a behavioral problem specific to only one situation been selected as the
focus of therapy.
Effects on Family Social Ecology
Fourth,
noncompliant behavior by the child may have indirect effects on family
functioning that may, in a reciprocal fashion, come back to have further
detrimental effects on the psychological adjustment of the defiant child. The
outcomes of impaired family management can be seen in Figure 6, as initially
demonstrated in the long-term program of research on aggressive children by
Gerald Patterson (1982) and subsequently supported through abundant research on
the outcomes of oppositional children (ODD). These outcomes are displayed in
Figure 6, below.
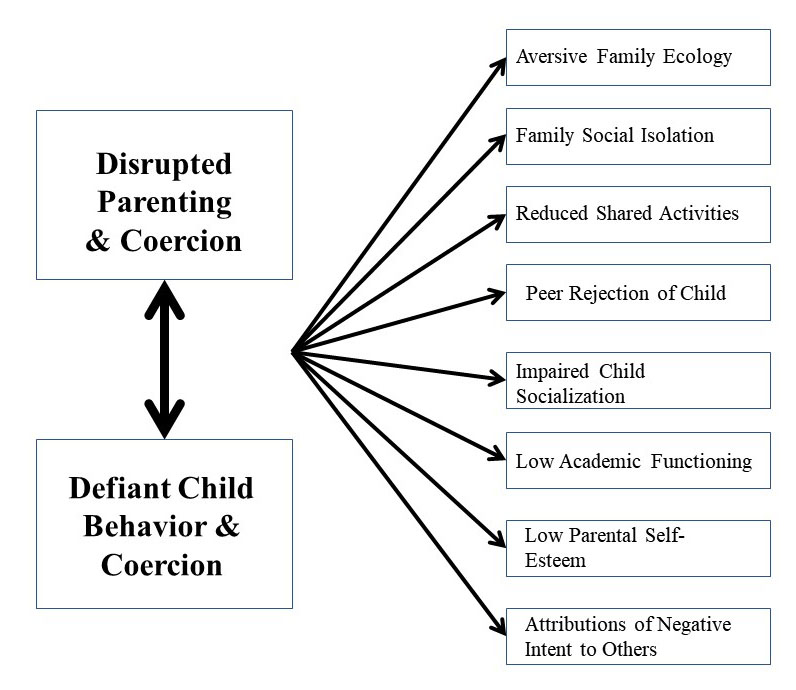
Figure 6. The potential outcomes of child defiant behavior, disrupted
parenting, and the coercive family process. From R. A. Barkley (2013). Defiant
Children: A Clinician’s Manual for Assessment and Parent Training (3rd ed.). New York: Guilford Press. Copyright 2013 by the Guilford Press.
Reprinted with permission.
As noted
already, out of this impaired family management process, the child rapidly
acquires a set of coercive behaviors to use against the parent and other family
members or even peers when the child is instructed to do something he/she does
not like to do. Parents may also come to acquire a set of rapidly escalating
coercive behaviors to use with the child because of those rare occasions where
yelling, threatening, or punishing the child has eventually led to compliance
by the child. Furthermore, over time parents may request progressively fewer
commands of the child, knowing in advance they will be met with resistant,
oppositional behavior by the child. Parents instead may assume more of the
child’s chores and responsibilities or assign them to a more compliant sibling.
The latter situation may then lead not only to declines in the child’s overall
level of successful adaptive functioning (i.e., independence, self-care, degree
of responsible conduct, etc.) and the child’s capacity to be socialized into
the larger community and society. Siblings may develop hostility and
resentment toward the defiant child because that child has comparatively less
work to do. In other cases, parents and siblings come to spend progressively
less leisure time and initiate fewer shared activities and recreational
pursuits with the defiant child so as to avoid any further difficulties with
that child. Siblings may also acquire and frequently utilize repertoires of
coercive behavior back toward the defiant child as well as toward parents, given that parents may frequently employ similar coercive tactics with other members of the family and not just the clinic-referred defiant child. Thus, the density of aversive social events within the families of defiant children is substantially higher than normal. That such family patterns might have negative effects on one’s self-esteem as a parent, on increasing the parent’s sense of helplessness, on family harmony, on marital harmony should the child oppose one parent more than the other, or on the self-esteem of the defiant child almost goes without saying and has been substantiated in research. And so there is a reciprocal system of effects existing within parent-child relations of defiant children where the behavior of parent and child affect each other bidirectionally while also resulting in broader “spillover” effects into the larger social ecology of the family.
Developmental Persistence
Fifth, noncompliance and defiant behavior in children appears to be highly stable over time, significantly predicting the persistence of this behavior pattern across development. Apart from ADHD with which it is often associated, childhood defiance or aggressiveness, in fact, may be one of the most stable of childhood behavioral disorders across development.
Prediction of Diverse Negative Developmental Outcomes
Targeting early defiant behavior for treatment is also important because of its repeated association in research with a variety of later maladjustments during the adolescent and young adult years. This is illustrated in Figure 1.3 as well. That is, defiant and coercive behavior, especially if it is of such magnitude and duration that it leads to referral for mental health services, is also a precursor or link to the development of other, more serious forms of antisocial behavior, criminal activity, and substance abuse. The pattern here is obvious; there is a developmental staging in the relationship of oppositional child behavior to later stages of physical aggression, status offenses, and crimes against property. Childhood oppositional behavior also significantly predicts later problems with academic performance and peer acceptance. The risk for later depression, suicidal ideation, and suicide attempts is also greater in children with defiant or aggressive behavior. Thus, research is coming to show that the presence of oppositional defiant behavior, or social aggression, in children is the most highly stable of childhood psychopathologies over development and is a more significant predictor of a widespread array of negative social and academic risks than are most other forms of deviant child behavior. These developmental risks become even more likely and more adverse when childhood defiant behavior is combined with higher levels of ADHD symptoms, particularly childhood impulsivity. Oppositional behavior is therefore singled out for treatment because of the significant potential it carries for future negative consequences for the child and family if left untreated.
A Prelude to Effective Treatment of Other Problems
Finally, it
would be hard to undertake the treatment of any other presenting problems of a
child without first addressing the child’s noncompliance. For example,
attempting to toilet train a 3-year-old noncompliant child is not likely to
prove successful until the child is taught to comply with requests. Similarly,
parental tutoring of a school-age child during homework performance is also
likely to fail as a consequence of the child’s reliance on defiant behavior
during work-related interactions with the parent. This will also be true of
noncompliant children who must adhere to other medical regimens or educational
programs in that such programs will likely prove less successful until the
child’s compliance with adult instructions is developed.
Implications of the Four Factor Model for Assessment
One
obvious implication of the model for assessing defiant children is that
clinicians must evaluate each factor represented in the model to fully
understand how a child may have come to be defiant, ODD, or socially aggressive
and, hopefully, what specific contributors exist within each factor that may
require attention and intervention.
Assessing Factor I: The Child’s Behavior and Related Disorders
The
evaluation of defiant children incorporates multiple assessment methods relying
on several informants concerning the nature of the children’s difficulties (and
strengths!) across multiple situations. To accomplish this, parent, child, and
teacher interviews are conducted, parent and teacher rating scales of child
behavior and rating scales or surveys of child adaptive functioning should be
obtained, and parent self-report measures of relevant psychiatric conditions
and of parent and family functioning also should be collected. Some clinicians
may wish to collect laboratory measures of ADHD symptoms, if that disorder is
present, as well as direct observations of parent-child interactions. And, of
course, children in whom intellectual or developmental delays or learning
disabilities are suspected should receive psychological testing of these
domains if such has not already been performed. For a more detailed discussion
of specific methods to use in evaluating oppositional children, see Defiant Children: A Clinician’s Manual for Assessment and Parent Training (Barkley, 2013), and more recently, Treating ADHD in Children and Adolescents: What Every Clinician Needs to Know (2022), which contains forms and rating scales that can be photocopied for use in the owner’s clinical practice.
Clinical
interviews provide a good starting point for gaining information on the nature
of defiant behavior a child may be demonstrating. But they are not normed and
so give no indication of the frequency or severity of such behavior relative to
a typically developing peer group of the same age and sex. For that end,
clinicians can use a broad band child behavior rating scale, such as the Child
Behavior Checklist (Achenbach, 2014) or the Behavioral Assessment System for
Children - (Reynolds & Kamphaus, 2015). These scales contain dimensions
that evaluate aggressive child behavior, among other dimensions of potential
psychopathology. If the clinician wants to examine the DSM-5 symptoms of ODD
specifically, then the clinical interview can be used for this purpose and the
recommended threshold of 4 of 8 symptoms that occur often can be used as the
determining cutoff for the presence of significant ODD symptoms. Defiant
behavior can also be evaluated using the Home Situations Questionnaire and
School Situations Questionnaire (see Barkley, 2013, 2022),
which have normative information for school-age children. Direct observations
of child behavior can be obtained in the clinic but these are often not
especially indicative of the nature of defiant behavior as it may occur in
natural settings in parent-child and teacher-child interactions. This is why
interviews and rating scales remain the best means of evaluating such behavior in a clinic referred child.
In general, there
are several goals to bear in mind in the evaluation of children for defiant
behavior. A major goal of such an assessment is not only the determination of
the presence or absence of psychiatric disorders, such as ODD, CD, and/or ADHD,
but also the differential diagnosis of ODD from other childhood psychiatric
disorders. This requires extensive clinical knowledge of these other
psychiatric disorders. In
evaluating defiant children, it may be necessary to draw on measures that are
normed for the individual’s country of residence that have a representative
sampling of the various ethnic backgrounds that exist in that general
population, if such instruments are available, so as to preclude the over-diagnosis
of minority children when diagnostic criteria developed from white children are
extrapolated to them.
Another
important purpose of the evaluation is the determination of comorbid conditions
and whether or not these may affect prognosis or treatment decision making. For
instance, the presence of high levels of physically assaultive behavior by the
child may signal that a parent training program such as this may be
contraindicated, at least for the time being, because of its likelihood of
temporarily increasing child violence toward parents when limits on
noncompliance with parental commands are established. Or consider the presence
of high levels of anxiety specifically and internalizing symptoms more
generally in children with ODD who may have ADHD as well. Research has shown
such symptoms to be a predictor of poorer responses to stimulant medication
or of a partial response than may be seen in
non-anxious children with ADHD. Similarly, the presence of high levels of irritable mood, severely
hostile and defiant behavior, and periodic episodes of serious physical
aggression and destructive behavior may be early markers for later severe mood
dysregulation disorder or, if accompanied with mood swings toward mania, even
childhood Bipolar Disorder (manic depression). Oppositional behavior is almost
universal in juvenile-onset Bipolar Disorder. Such
a disorder will likely require the use of psychiatric medications in
conjunction with a parent training program.
A further
objective of the evaluation is to identify the pattern of the child’s
psychological strengths and weaknesses and to consider how these may affect
treatment planning. This may also include gaining an impression of the parents’
own abilities to carry out the treatment program, as well as the family’s
social and economic circumstances and the treatment resources that may (or may
not) be available within their community and cultural group. Some determination
will also need to be made as to the child’s eligibility for special educational
services within his/her school district, if eligible disorders, such as
developmental delay, learning disabilities, or ADHD, are present.
A final purpose
of the evaluation is to begin delineating the types of interventions that will
be needed to address the psychiatric disorders and psychological, academic, and
social impairments identified in the course of assessment. As noted later,
these interventions may include individual counseling, parent training in
behavior management, family therapy, classroom behavior modification,
psychiatric medications, and formal special educational services, to name just
a few.
As the foregoing
discussion illustrates, the evaluation of a child for the presence of defiant
behavior is but one of many purposes of the clinical evaluation of ODD
children.
Assessing Factor II: Disrupted Parenting
As
the explanation of the four-factor model made evident, disrupted parenting is
frequently a major contributor to oppositional behavior and, in concert with
the child’s features discussed above, creates the final common pathway for the
generation of noncompliant and defiant behavior. Although some rating scales
of parenting exist in research articles, they are not normed on a U.S.
population and so are not relevant to the clinical evaluation of an individual
case. The Home and School Situations Questionnaires noted above (see Barkley, 2013, 2022) can help to evaluate those situations in which a child is displaying uncommon levels of defiant behavior but are not able to capture the nature of the parent’s own part of these interactions. For that purpose, I recommend following up those rating scales (when completed) with an interview with the parents. This interview would involve discussing each of the situations on the left hand side of this table. If parents indicate this situation is a problem, then use the questions on the right hand side to probe for the specific nature of the parent-child interactions in this situation. The clinician is seeking here to identify a pattern of inconsistent, vacillating (harsh vs. lax), emotional, and generally ineffective parenting as described in detail in the model above.
Parental Interview Format for Assessing
Child Behavior Problems at Home and in Public |
Situation to be discussed |
If a problem, follow-up questions to ask |
Overall parent-child interactions
Playing alone
Playing with other children
Mealtimes
Getting dressed/undressed
Washing and bathing
When parent is on telephone
When child is watching television
When visitors are in your home
When you are visiting someone else’s home
In public places (stores, restaurants, church, etc.)
When father is in the home
When child is asked to do chores
When child is asked to do school homework
Bedtime
When child is riding in the car
When child is left with a babysitter
Any other problem situations |
1. Is this a problem area? If so, then proceed with questions 2-9.
2. What does the child do in this situation that bothers you?
3. What is your response likely to be?
4. What will the child do in response to you?
5. If the problem continues, what will you do next?
6. What is usually the outcome of this situation?
7. How often do these problems occur in this situation?
8. How do you feel about these problems?
9. On a scale of 1 (no problem) to 9 (severe), how severe is this problem
for you? |
From Barkley (1981, p. 98; 1987, 1997a, 2022). Copyright
1981, 1987, 1997 by The Guilford Press. Reprinted by permission.
Assessing Factor III: The Parent’s Psychological Status
It is apparent from
the four-factor model that child defiant behavior and related disorders such as
ODD, their level of severity, and their response to interventions are, in part,
a function of factors affecting parents. As noted above, several types of
psychiatric disorders are likely to occur more often among family members of a
child with defiant behavior or ODD than in matched groups of control children.
That these problems might further influence the frequency and severity of
behavioral problems in defiant children has been demonstrated in numerous
studies over the past 20 years. Also noted earlier is the fact that the extent
of social isolation in mothers of behaviorally disturbed children influences
the severity of the children’s behavioral disorders as well as the outcomes of
parent training. Others have also shown parental psychopathology and marital
discord separately and interactively contribute to the decision to refer
children for clinical assistance, the degree of conflict in parent-child
interactions, and child antisocial behavior. The degree of resistance of
parents to parent training is also dependent on such factors. Assessing the
psychological integrity of parents, therefore, is an essential part of the
clinical evaluation of defiant children, the differential diagnosis of their
prevailing disorders, and the planning of treatments stemming from such
assessments. Thus, the evaluation of children for defiant behavior is often a
family assessment rather than one of the child alone. Although space does not
permit a thorough discussion of the clinical assessment of adults and their
disorders, brief mention will be made of some assessment methods that
clinicians have found useful in providing at least a preliminary screening for
certain important variables in the treatment of defiant children.
The instruments
that assess the parents’ own adjustment, discussed below, can be completed by
parents in the waiting room during the time their child is being interviewed.
They should not mailed out in advance with the other rating scales, as the
clinician will need to introduce the purpose of these self-report scales
briefly to the parents so as not to offend them with the request for such
sensitive information. Typically, I have indicated to parents that having a
complete understanding of a child’s behavior problems requires learning more
about both the children and their parents. This includes gaining more
information about the parents’ own psychological adjustment and how they view
themselves in their role as parents. The rating scales below are then
introduced as one means of gaining such information. Few parents refuse to
complete these scales after an introduction of this type. To save time, some
professionals prefer to send these self-report scales out to parents in advance
of their appointment, at the same time as the child behavior questionnaires. If
so, be sure to prepare a cover letter that sensitively explains to parents the
need for obtaining such information about the parent. For instance, this letter
might include the following statement:
“When completing
the questionnaires pertaining to yourself and to other aspects of your marriage
and family, please keep in mind that we are not trying to evaluate you.
Instead, we are trying to learn as much as we can about the home environment in
which your child lives. That home environment is very important in helping to
understand the nature of the problems a child may be experiencing. Having such
information allows us to make careful and well-informed recommendations about how
best to help your child become more successful and better adjusted both at home
and at school.”
Parental ADHD and ODD
Family studies of the aggregation of psychiatric disorders among the biological relatives of children with ADHD and ODD have clearly demonstrated an increased prevalence of ADHD and ODD among the parents of these children. In general, there seems to be at least a 40-50% chance that one of the two parents of the defiant child with ADHD will also have adult ADHD (15-20% of mothers and 25-30% of fathers). The manner in which ADHD in a parent might influence the behavior of an ADHD child specifically and the family environment more generally has not been well studied. Adults with ADHD have been shown to be more likely to have problems with anxiety, depression, personality disorders, alcohol use and abuse, and marital difficulties; to change their employment and residence more often; and to have less education and lower socioeconomic status than adults without ADHD. Greater diversity and severity of psychopathology among parents is particularly apparent among the subgroup of ADHD children with comorbid ODD or CD. More severe ADHD seems to also be associated with younger age of parents, suggesting that pregnancy during their own teenage or young adult years is more characteristic of parents of ADHD than non-ADHD children. It is not difficult to see that these factors, as well as the primary symptoms of ADHD, could influence the manner in which child behavior is managed within the family and the quality of home life for such children more generally. Research suggests that where the parent has ADHD, the probability that the child with ADHD will also have ODD increases markedly. Other studies indicate that ADHD in a parent may interfere with the ability of that parent to benefit from a typical behavioral parent training program. Treatment of the parent’s ADHD (with medication) may result in greater success in subsequent retraining of the parent. These preliminary findings are suggestive of the importance of determining the presence of ADHD and even ODD in the parents of children undergoing evaluation for these disorders.
Recently, the
DSM-IV symptom list for ADHD have been cast in the form of a behavior rating
scale, and U.S. norms on more than 1,200 adults, ages 17 to 81-years-old, have been
collected. Given that DSM-5 has made no changes to these
symptoms, the scale is just as applicable to evaluating parents for a possible
DSM-5 diagnosis of ADHD. This rating scale for adults, entitled the Barkley
Adult ADHD Rating Scale is completed twice; once for their current
behavioral adjustment and a second time for their recall of their childhood
behavior between ages 5 to 12-years-old. Norms for both current and childhood recall
scores are provided in the manual. Clinically significant scores on these
scales do not, by themselves, ensure the diagnosis of ADHD in a parent but
should raise suspicion in the clinician’s mind about such a possibility. If so,
consideration should be given to referral of the parent for further evaluation
and, possibly, treatment of adult ADHD, if necessary.
The use of such
scales in the screening of parents of defiant children would be a useful first
step in determining if the parents had ADHD. If the child meets diagnostic
criteria for ADHD and these screening scales for ADHD in the parents proved
positive (clinically significant), then referral of the parents for a more
thorough evaluation and differential diagnosis might be in order. At the very
least, positive findings from the screening would suggest the need to take them
into account in treatment planning and parent training.
Parental Psychological Difficulties
Parents of
defiant children are frequently more depressed than those of normal children
and this may affect their responsiveness to behavioral parent training
programs. A scale often used to provide a quick assessment of parental
depression is the Beck Depression Inventory (Beck, Steer, & Garbin, 1988).
Greater levels of psychopathology generally and psychiatric disorders
specifically also have been found in parents of children with ADHD, many of
whom also have ADHD. One means of assessing this area of parental difficulties
is through the use of the Symptom Checklist 90 – Revised (SCL-90-R; Derogatis,
1994). This instrument not only has a scale assessing depression in adults but
also scales measuring other dimensions of adult psychopathology and
psychological distress. Whether clinicians use this or some other scale, the
assessment of parental psychological distress generally and psychiatric
disorders particularly makes sense in view of their likely impact on parenting
and child defiant behavior as well as on the course and the implementation of
the child’s treatments, typically delivered via the parents.
Assessing Factor IV: Family Background and Stress Events
Certainly,
clinical interviews can be used to evaluate possible background stressful or
other life events that might have some impact on disrupting parenting and
generating child defiant behavior. Unemployment, financial problems, marital
difficulties, chronic health problems, tense or conflict-ridden interactions
with extended family, and other factors are worth exploring in such an
interview to gain some idea of their salience in a specific case. A few rating
scales can be useful supplemental methods to this part of the clinical
interview.
Parental
Stress: Research as early as 25 years ago suggested that parents of
behavior problem children, especially those children with comorbid ODD and
ADHD, report more stress in their families and their parental role than those
of normal or clinic-referred non-ADHD children. One measure frequently used in
such research to evaluate this construct has been the Parenting Stress Index
(PSI; Abidin, 1995). The current PSI is a 120-item multiple choice
questionnaire, which can be scored to yield six scores pertaining to child
behavioral characteristics (e.g., distractibility, mood, etc.), eight scores
pertaining to maternal characteristics (e.g., depression, sense of competence
as a parent, etc.), and two scores pertaining to situational and life stress
events. These scores can be summed to yield three domain or summary scores, these
being Child Domain, Mother Domain, and Total Stress. A shorter version of this
scale is available and clinicians are encouraged to utilize it
in evaluating parents of defiant children.
Marital
Discord: Many instruments exist for evaluating marital discord
between parents. The one most often used in research on childhood disorders has
been the Locke-Wallace Marital Adjustment Scale (Locke & Wallace, 1959). As
noted above, marital discord, parental separation, and parental divorce
are more common in parents of defiant children. Parents with such marital
difficulties may have children with more severe defiant and aggressive behavior
and such parents may also be less successful in parent training programs. Screening parents for marital problems, therefore, provides
important clinical information to therapists contemplating a parent training
program for such parents. Clinicians are encouraged to incorporate a screening
instrument for marital discord into their assessment battery.
Implications of the Four Factor Model for Treatment
When Is Treatment Justified?
Some
minor amounts of noncompliant or defiant behavior is normal for children,
particularly those in the preschool age group, and should not be thought of as
being pathological or abnormal just because it may occur sporadically. Nor will
such typical and occasional defiance justify a clinical treatment program such
as this one. In my opinion clinicians must take care to establish at least
two of the following three criteria for determining that the noncompliant
behavior shown by a child referred to them can be justified as in need of
clinical intervention:
1. The
child’s behavior is developmentally inappropriate or statistically deviant in
that it occurs to a significantly greater degree than is common for children of
this age group. This can be established through the use of child behavior
rating scales that include this dimension of behavior, often called aggression
or conduct problem by scale developers. Suffice it to say that the child’s behavior
should be rated as falling at least above the 84th percentile (1 standard
deviation [SD] above the mean) or higher on such rating scales in order
to establish such deviance. Although this information will typically be
obtained through the use of parent reports of the child’s behavior because the
home setting is where such behavior is usually at its worst, teacher reports on
these rating scales may also be used to establish this criterion of
developmental inappropriateness. Alternatively, through clinical interview with
the parent one can discover whether the child demonstrates sufficient symptoms
of ODD or CD as to meet clinical criteria for either of these diagnoses as
established in DSM-5 (American Psychiatric Association, 2013).
2. The
child’s behavior is resulting in an appreciable degree of impairment. That is,
the behavior pattern is interfering with the child’s capacity to function
effectively in various domains of major life activities. This means that the
child does not meet appropriate developmental expectations for adaptive
behavior, such as self-care, or for appropriate social interaction with family
members and peers, acceptance of age-appropriate responsibilities as in chore
and homework performance, school functioning, and the capacity to be trusted to
adhere to rules in the absence of immediate caregiver (typically parental)
supervision, among other domains. Such levels of impairment can be established
to a limited degree using some child behavior rating scales completed by
parents and teachers that have questions dealing with adaptive behavior in
major domains of life, such as the Child Behavior Checklist
or Behavior Assessment System for Children - 2 or through interviews and inventories with parents that
explicitly assess adaptive functioning, such as the Vineland Adaptive Behavior
Scale, the Normative Adaptive Behavior Scale, or other such instruments. More specifically, clinicians may wish to use
the Barkley Functional Impairment Scale - Children and Adolescents (Barkley,
2012a) that covers parent reports of child impairment in more domains of major
life activities (15) than other child behavior rating scales and has current
nationally representative norms for children ages 6-17 years. For our purposes,
establishing that a defiant child is impaired means that they place at or below
the 7th-10th percentile for his/her age on one of these
well-normed rating scales of impairment.
3. The
child’s behavior is resulting in a significant degree of emotional distress or
harm, either for the child or, more likely, for the parents. Child distress may
be established through the use of child self-report measures of emotional
adjustment, such as ratings of or interviews about anxiety or depression, that
convey an impression of the child’s unhappiness with the current state of
affairs in the family specifically or their social adjustment more generally.
Parent distress may be readily established most directly through the use of
parent self-report instruments designed to measure this domain, such as the
Short Form of the Parenting Stress Index (Abidin, 1991).
Regardless of the specific methods used to evaluate these intervention criteria, the clinician must make some effort to demonstrate that the child’s defiant behavior pattern is outside the bounds of normally appropriate child conduct and that it is impairing the child’s adjustment in some way or is creating distress for the child, the caregiver, or others and thus is in need of clinical intervention. Statistical deviance of a child’s behavior alone may not justify either clinical diagnosis or clinical intervention. It may be helpful here to consider the related issue of what defines a behavior pattern as a mental disorder, out of which may come some guidance concerning the issue of when to treat. As discussed by Wakefield (1992), the clinician is attempting to establish that a “harmful dysfunction” exists and is deserving of a label of mental disorder and/or clinical treatment. Wakefield (1992) goes further and requires that an aberration in an internal, normal psychological or cognitive mechanism must also be present to define a “harmful dysfunction”; this must be shown before a diagnosis of mental disorder is rendered. Some defiant or antisocial children may show no evidence of aberrant cognitive mechanisms, although many do particularly in the domain of emotional self-regulation, and their deviant behavior may arise as a result of external mechanisms, such as disrupted, disadvantaged, or even criminogenic environments. Such children without evidence of a deficient cognitive or psychological mechanism may not be viewed as having mental disorders by Wakefield’s definition. Others disagree with Wakefield’s criterion of an aberrant cognitive mechanism (Lilienfeld & Marino, 1995), however, and argue that “fuzzy” boundaries will invariably exist between normality and abnormality by virtue of the dimensional nature of individual psychological characteristics and behaviors and because one must make arbitrary choices about “where to carve nature at her joints” to define abnormality along any dimension. Also, I am not sure that a criterion of an aberrant internal mechanism or even a diagnosis of mental disorder is needed to justify the use of psychosocial treatment for the child and his/her parent. Some relatively socially benign interventions, such as parent training in child management, may be justifiable even though some children whose parents undergo such training do not meet diagnostic thresholds for a mental disorder or Wakefield’s complete criteria for a “harmful dysfunction.” The implementation of treatment, in other words, may not necessarily depend on a diagnosis of a mental disorder, although often it does, but should instead be focused on the reduction of impairment or harm even if no cognitive dysfunction is evident.
In the end, what
all of this means is that the clinician must stay alert to the occasional
possibility that some children and their families do not need training in specific
child management skills. This may result from the fact that some parents, by
dint of their own psychological or psychiatric disorders, are significantly
distressed by even normal, garden-variety child misbehavior or noncompliance.
In such cases, the parents may need intervention for changing their own
distress (and developmental expectations of children) or addressing their own
psychological disorder rather than the child’s behavior needing clinical
treatment. Milder instances of this phenomenon, where parents manifest no
serious psychological disorders, may simply reflect an excess of parental
concern about their children’s adjustment and their own competence as parents.
In these cases, the clinician may only need to offer simple reassurance that
all seems well with the child and that the parent seems to be doing a
reasonable job of parenting. Likewise, some children may show higher than
normal levels of oppositional behavior that do not achieve clinically
significant levels of deviance, result in no distress for the parent or child,
or are not associated with significant impairment in major life activities. Such
children may be viewed as more stubborn, “pig-headed,” strong-willed,
temperamental, rigid, or opinionated but such personality descriptors alone
would not justify clinical intervention. And there certainly exist those rare
cases of children who may be distressed by their own social conduct, even
though not clinically deviant in their noncompliance, not distressing to their
parents, or/and not impairing of a major domain of life activity, as in the
case of social phobia, major depressive disorder, dysthymic disorder, or even
obsessive-compulsive disorder. Such children may well be in need of clinical
treatment for their own psychological distress but not specifically in need of
a parent training program aimed at noncompliant child behavior management as that
described here. But the presence of at least two of the three criteria set
forth above is likely to indicate that a child’s behavior is placing him/her at
significant risk for current and later maladjustment or risk for other
disorders, social and academic failure, antisocial activities, and other
significant negative developmental outcomes. This establishes that a “harmful
dysfunction” exists (even if not associated with an aberrant cognitive
mechanism) and that such risks justify clinical intervention.
Addressing Factor I: Childhood Psychological Disorders
Through the
evaluation, the clinician has gained some indication of what pre-existing
childhood characteristics exist that might be contributing to defiant behavior
and parent-child conflict. Among these, the most common is likely to be ADHD,
although major depression, bipolar disorder, disruptive mood dysregulation disorder, psychopathic personality, among
other disorders may also be contributing factors. Treatments for these
disorders, including psychiatric medication, may be needed apart from any
program of parent training that is going to be implemented. Indeed, failure to
address these disorders may well contribute to subsequent failure of such a
training program.
Addressing Factor II: Disrupted Parenting
This course has
shown you that there are several important aspects of the parent-child
interactions of oppositional children that have implications for the training
of such parents in effective child management procedures. The most important
are that parents must be trained to:
(1) increase the
value of their attention generally, and its particular worth in motivating and
reinforcing their child’s positive behavior;
(2) increase the
positive attention and incentives they provide for compliance while decreasing
the inadvertent punishment they provide for occasional compliance;
(3) decrease the
amount of inadvertent positive attention they provide to negative child
behavior;
(4) increase the
use of immediate and consistent mild punishment for occurrences of child
noncompliance;
(5) ensure that
escape from the activity being imposed upon the child does not occur (i.e., the
command is eventually complied with by the child);
(6) reduce the
frequency of repeat commands parents employ so as to avoid delays to
consequences (act, don’t yak);
(7) recognize
and rapidly terminate escalating and confrontational negative interactions with
the child; and
(8) ensure that
the parents do not regress to a predominantly punitive child management
strategy once training has been completed.
All of this,
then, should serve to reduce the unpredictability involved in indiscriminant or
inconsistent parenting while ensuring that child’s coercive oppositional
behaviors are unsuccessful in their function to escape or avoid parental
requests, demands, and commands.
Addressing Factors III and IV: Parent Psychological Difficulties and
Family Distress
Just as with
Factor I, the clinician may need to recommend various treatments for any parent
psychological and psychiatric disorders detected in the evaluation. In ODD
children, especially where ADHD is a comorbidity, parental ADHD, among other
disorders, is likely to be found in a substantial minority of parents. As
noted above, substance use disorders, depression, or anxiety disorders may also
be more likely. Hence parents may require interventions for their own disorders
prior to or concomitant with any parent training program so as to maximize the
likelihood of also reducing parent-child conflict and child defiant behavior.
Also, to the extent that various family stress events may exist, referral for
social services assistance, medical evaluation and treatment, marital therapy,
or other interventions may be called for in dealing with particular stress
events identified during the evaluation.
There are numerous well-studied Behavioral Parent Training programs (BPT) available through commercial sources, and their respective clinical manuals or the books written for a parent audience are quite adequate for teaching the techniques. The most commonly used programs having some evidence for their effectiveness are:
- Defiant Children (Barkley)
- Community Opportunities for Parent Education (Cunningham)
- Parent-Child Interaction Therapy (PCIT) (Eyberg)
- The Incredible Years Program (Webster-Stratton)
- Positive Parenting Practices (PPP) (Sanders)
- Parents are Teachers (Becker)
- The Noncompliant Child (Forehand and McMahon)
- New Forest Parenting Program (Thompson)
- Parenting Hyperactive Preschoolers (Harvey)
- Treating Explosive Kids (Greene & Ablon)
Many of these programs have been around for decades. The programs by Webster-Stratton, Thompson, and Harvey are targeted mainly at preschool children. The others encompass a wider age range up to adolescence. There has been little innovation in these methods over that time except for two programs. One was the development of the program explicitly intended for preschool children with ADHD called the New Forest Program by Thompson and colleagues in Europe and a different program for that age group by Harvey in the United States. Those programs focus to some extent on ADHD-specific symptoms, such as inattention, and with preschool children, but they also convey general behavior management strategies as do traditional BPT programs. The other programs are for conduct or behavioral problem children and can be used up until adolescence. They focus more on parent-child conflict, compliance, and improving parental consistency of consequences as described below.
The program by Green and Ablon does not focus so much on contingency management following traditional operant conditioning principles. Instead, it teaches parents collaborative problem solving in which the child is actively invited into brainstorming possible ways of resolving parent-child conflicts so as to reach agreement with parents on a resolution of the problem. Only two studies to date by the developer have been published, both from the same single project. They showed little or no advantage of this approach over traditional BPT (my program specifically) for improving child conduct problems although some parents reported greater acceptability of the problem-solving methods being taught.
To these programs, some developers add other parent exercises focused on building up a better relationship with the child or more positive attachment. This is often done through nondirective play periods several times per week in which parents simply comment positively or otherwise attend to ongoing positive child play behavior, as in my program. Research has shown such relationship building is not necessary for families who seek assistance with problem behaviors in primary care, school, or other community service settings that are not specifically mental health or psychiatric clinics. That is because the child’s problems usually have not reached such an extreme stage that the parent-child relationship is primarily negative. But by the time parents may seek assistance from secondary or tertiary level mental health settings, which are the settings in which I usually practiced, these relationship-focused exercises were important and effective to teach as the parent-child relationship had grown quite conflicted and negative.
Training Parents of Defiant Children in Behavior Management Methods
All of the eight important issues described above in which parents require training are addressed in my program, Defiant Children. It consists of 10 steps, with 1 to 2 hour weekly training sessions provided either to individual families or in groups. Each step is described in detail in the clinical manual (see References). Assessment tools and parent handouts are also provided in the manual and can be photocopied for use in the owner’s clinical practice. The program is briefly presented below:
1. Review of Information on ADHD (if necessary)
In the first session, the therapist provides a succinct overview of the nature, developmental course, prognosis, and etiologies of ADHD. Providing the parents with additional reading materials, such as an accompanying trade book for parents (Your Defiant Child), can be a useful addition to this session. Professional DVDs are also available that present such an overview and can be loaned to parents for review at home and sharing with relatives or teachers, as needed. Such a session is essential in parent training to dispel a number of misconceptions parents often have about ADHD in children. Research suggests that just this provision of information can result not only in improved knowledge of parents about ADHD but also in improved parental perceptions of the degree of deviance of their child’s behavioral difficulties.
2. The Causes of Oppositional/Defiant Behavior
Next, parents are provided with an in-depth discussion of those factors identified in past research as contributing to the development of defiant behavior in children. Essentially, four major contributors are discussed, these being: (a) Child characteristics, such as health, developmental disabilities, and temperament; (b) Parent characteristics similar to those described for the child; (c) Situational consequences for oppositional and coercive behavior; and (d) Stressful family events. Parents are taught that where problems exist in (a), (b), and (d), they increase the probability of children displaying bouts of coercive, defiant behavior. However, the consequences for such defiance, (c) above, seem to determine whether that behavior will be maintained or even increased in subsequent situations where commands and rules are given. Such behavior appears to primarily function as escape/avoidance learning in which oppositional behavior results in the child escaping from aversive parent interactions and task demands, negatively reinforcing the child's coercion. As in the first session, this content is covered so as to correct possible misconceptions that parents have about defiance (e.g., it is primarily attention-getting in nature). This session can be augmented by the use of two of my professional DVDs on the nature of oppositional defiant behavior and its management (Understanding-the-Defiant-Child; Managing-the-Defiant-Child).
3. Developing and Enhancing Parental Attention
Gerald Patterson suggested that the value of verbal praise and social reinforcement to oppositional or hyperactive children is greatly reduced, making it weak as a reinforcer for compliance. In this session, parents are trained in more effective ways of attending to child behavior so as to enhance the value of their attention to their children. The technique consists of verbal narration and occasional positive statements to the child with attention being strategically deployed only when appropriate behavior is displayed by the child. Parents are taught to reduce the amount of attention to inappropriate behaviors, including ignoring as much negative behavior as possible, while greatly increasing their attention to ongoing prosocial and compliant child behaviors. This is a critical step because many parenting programs result in reductions of rates of negative behavior without corresponding increases in rates of positive behavior. One of the most effective results of parent training is to increase rates of positive behaviors that are incompatible with the negative behaviors the parents wish to terminate.
4. Attending to Child Compliance and Independent Play
This session extends the techniques developed in Session 3 to instances when parents issue direct commands to children. Parents are trained in methods of giving effective commands, such as reducing question-like commands (e.g., Why don't you pick-up your toys now?), increasing imperatives, eliminating sitting activities which compete with task performance (e.g., television), and reducing task complexity. Parents are then encouraged to begin using a more effective commanding style and to pay immediate positive attention when compliance is initiated by the child. As part of this assignment, parents are asked to increase the frequency with which they give brief commands to their child this week and to reinforce each command obeyed. Research suggests that these brief commands are more likely to be obeyed thereby providing excellent training opportunities for attending to compliance. In this session, parents are also trained to provide more positive attention frequently and systematically when their children are engaged in nondisruptive activities while parents must be occupied with some other work or activity. Essentially, the method taught here amounts to a shaping procedure in which parents provide frequent praise and attention for progressively longer periods of child nondisruptive activities.
5. Establishing a Home Token Economy
As noted above in discussing the theoretical model of ADHD, children with the disorder may require more frequent, immediate, and salient consequences for appropriate behavior and compliance in order to maintain it. If this is correct, then instituting a home token economy is critical to addressing these difficulties with intrinsically generated and represented motivation, by bringing more salient external consequences, more immediately, and more frequently to bear on child compliance than is typically the case. In establishing this program, the parents list most of the children's home responsibilities and privileges and then assign values of points or chips to each. The parents are encouraged to have at least 12 to 15 reinforcers on the menu so as to maintain the motivating properties of the program. Generally, plastic chips are used with children 8 or younger as they seem to value the tangible features of the token. For 9 year olds or older, points recorded in a notebook seem sufficient.
During the first week of this program, the parents are not to fine the child or remove points for misconduct. The program is for rewarding good behavior only. Parents are also asked to be liberal in awarding chips to children for even minor instances of appropriate conduct. However, chips are given only for obeying first requests. If a command must be repeated, it must still be obeyed but the opportunity to earn chips has been forfeited. Parents are also encouraged to give bonus chips for a good attitude or emotional regulation in their children. For instance, if a command is obeyed quickly, without complaint, and with a positive attitude, parents may give the child additional chips beyond those typically given for that job. Where this is used, parents are to expressly note that the awarding of the additional chips is for a positive attitude. Families are encouraged to establish and maintain such programs for at least 6 to 8 weeks to allow for the newly developed interaction patterns spawned by such programs to become habitual patterns in dealing with child compliance.
6. Implementing Time Out for Noncompliance
Parents are now trained to use response cost (removal of points or chips) contingent on noncompliance. In addition, they are trained in an effective time-out-from-reinforcement technique for use with two serious forms of defiance that may continue to be problematic despite the use of the home token economy. These two misbehaviors are selected in consultation with the parents and typically involve a type of command or household rule that the child continues to defy despite parental use of previous treatment strategies. Time out is limited to these two forms of misconduct so as to keep it from being used excessively during the next week.
The time out procedure taught to parents often differs from that commonly used by them. First, the time out is to be implemented shortly after noncompliance by a child begins. Parents often wait until they are very upset with a child before instituting punishment, often repeating their commands frequently to a child in the interim. In this program, parents issue a command, wait 5 seconds, issue a warning, wait another 5 seconds, and then take the child to time out immediately should compliance not have begun to these commands or warnings. Second, children are not given control over the time out interval as they often are in many households. For instance, parents often place a child in time out then say the child can leave time out when they are quiet, ready to do as the parent asked, or when a timer signals the end of the interval. In each of these cases, determination as to when the time out interval ends is no longer under the parent’s control. This program teaches parents to simply tell the child to not leave the time out chair until the parent tells them to. Three conditions must be met by the child before time out ends and these are in a hierarchy: (1) The child must serve a minimum sentence in time out, usually 1 to 2 minutes for each year of their age; (2) the child must then become quiet for a brief period of time so as not to have disruption associated with the parents approaching the time out chair and talking to the child; and (3) the child must then agree to obey the command. Failure of the child to remain in time out until all three conditions are met is dealt with by additional punishment. The consequence is tailored to meet parental wishes but may consist of a fine within the home token system, extension of the time out interval an additional 5 or 10 minutes, or placement of the child in his or her bedroom. In the latter case, toys or other entertaining activities are previously removed from the bedroom and the door to the room may be closed and locked to preclude further escape from the punishment.
7. Extending Time Out to Additional Noncompliant Behaviors
In this session, no new material is taught to parents. Instead, any problems with previously implementing time out are reviewed and corrected. Parents may then extend their use of time out to one or two additional noncompliant behaviors with which the child may still have trouble.
8. Managing Noncompliance in Public Places
Parents are now taught to extrapolate their home management methods to troublesome public places, such as stores, church, restaurants, etc. Using a "think aloud-think ahead" paradigm, parents are taught to stop just before entering a public place, review two or three rules with the child which the child may previously have defied, explain to the child what reinforcers are available for obedience in the place, then explain what punishment may occur for disobedience, and finally assign the child an activity to perform during the outing. Parents then enter the public place and immediately begin attending to and reinforcing ongoing child compliance with the previously stated rules. Time out or response-cost are two methods used immediately for disobedience.
Time out in a public place may require slight modification from its use at home. For instance, parents may be taught to stand the child against the farthest wall from the central aisle of a store to serve as the time out location. If inconvenient, then taking the child to a restroom or having him face the side of a display cabinet may be adequate substitutes. If unavailable, then taking the child outside the building to face the front wall or returning to the car can be used for time out. When none of these locations seem appropriate, parents can be trained to use a delayed punishment contingency. In this case, the parent carries a small spiral notebook to the public place and, before entering the building, indicates that rule violations will be recorded in the book and the child will serve time out for them upon return home from this trip. This author encourages parents to keep a picture of the child sitting in time out at home with this notebook and to show it to the child before entering the public building. This serves as a reminder to the child of what may be in store should a rule be violated. Whenever time out is used in a public place, it need not be for as long an interval as at home. The author suggests that that half of the usual time out interval may be sufficient for public misbehavior given the richly reinforcing activities in public places from which the child has just been removed.
9. Improving Child School Behavior From Home
The Daily School Behavior Report Card: This session was designed to help parents assist their child’s teacher with the management of classroom behavior problems. The session focuses on training parents in the use of a home-based reward program. Children are evaluated on a daily school behavior report card by their teachers. This card serves as the means by which consequences later in the day will be dispensed at home for classroom conduct. The card can be designed to address class behavior, recess or free time behavior, or more specific behavioral or academic targets for any given child. The consequence provided at home typically consists of the rewarding or removal of tokens or points within the home token system as a function of the ratings the child has received from their teachers on this daily behavioral report card. To emphasize the importance of the school to home communication and to avoid escaping consequences if the child “loses” their school behavior report card, it is best to set up a contingency such that “no news is worse than bad news.” Thus, the most austere level in the contingency system should be when the card is incomplete or missing.
10. Managing Future Misconduct
By now, parents should have acquired an effective repertoire of child management techniques. The goal of this session is to get parents to think about how they might be implemented in the future if some other forms of noncompliance developed. The therapist challenges the parents with misbehaviors they have not seen yet and asks them to explain how they might use their recently acquired skills to manage these problems. Behavioral rehearsal (i.e., role plays) surrounding anticipated barriers to implementation of existing parenting plans or making modifications or innovations to deal with new and different behaviors are strongly recommended as a means to prepare for future misconduct.
One Month Review/Booster Session
In what is typically the final session, the concepts taught in earlier sessions are briefly reviewed, problems which have arisen in the last month are discussed, and plans made for their correction. Other sessions may be needed to deal with additional issues that persist but for most families, the previous 10 sessions appear adequate for improving rates of compliant behavior in ADHD children.
The program is intended for children ages 2 to 11 years where oppositional or defiant behavior is an issue. Studies examining the efficacy of this particular BPT with ADHD children have consistently reported significant improvements in child behavior as a function of the parents’ acquisition of these child management skills. Indeed, this was the program that was selected, and modified, for use in the large-scale NIMH Multimodal Treatment of ADHD study (see my other course, ADHD in Children: Diagnosis, Assessment and Management). Results suggest that up to 64 percent of families experience clinically significant change or recovery (normalization) of their child’s disruptive behavior as a consequence of this program. However, improvements in behavior may be more concentrated in the realm of aggressive and defiant child behavior than in inattentive-hyperactive symptoms. All of these studies have relied on clinic-referred families most of whom sought the assistance of mental health professionals for their children.
In contrast to the results of research with such motivated families, I and colleagues found that if such a clinic-based parent training program is offered to parents whose preschool children were identified at kindergarten enrollment as having significant levels of aggressive-hyperactive-impulsive behavior, most do not attend training or do not attend reliably and no treatment effect is evident. Moreover, no significant improvements in child behavior were found even among those who did attend at least some of the training sessions. Studies with disruptive children or those at high risk for externalizing behavior suggest that BPT may be more cost-effective, reach more severely disruptive children and more minority families, and possibly be more effective for them if they are provided as group training classes offered through neighborhood public schools in the evenings using para-professionals as trainers. This might prove to be the case for children specifically having ADHD as well.
Program Effectiveness and Predictors of BPT Success
The effectiveness of BPT declines with age of the child, such that it is most effective in early childhood (65%–75% positive response) and remains at that level through elementary school. But by 12–14 years of age, it declines to about a 25%–35% response rate. That is still better than traditional approaches to family therapy but is just a third of the response rate for young children. Such a fall-off in benefit is not unexpected when one considers that adolescents are psychologically and socially individuating from their parents, parental influence over them declines markedly, peer influence and other out-of-home effects become more prominent in their influence, and genetic differences in personality and especially psychopathology become more prominent as influences on family relationships and teen disruptive behavior.
What factors predict success in these programs?
- Parental motivation to attend BPT. Parents who neither requested BPT (as in community screenings identifying high risk or ADHD/ODD children) nor seem interested in receiving it (when offered by clinicians after an evaluation of their child) are not good candidates as most of the former families and 28%+ of the latter will not attend any sessions even if it is free of charge.
- Parental Psychological Disorder. Parental ADHD significantly increases risk for failure in BPT, as does parental depression and substance use disorders. Yet evidence is mixed as to whether treating parental ADHD with medication results in improved participation in BPT. These disorders still need to be managed before or concurrent with the use of BPT to offer the chance to at least try to increase the likelihood of a positive response to BPT.
- Chronic health problems in the parent, such as chronic fatigue syndrome, etc. These problems make it harder to apply these methods consistently, suggesting that, where possible, the unaffected parent take on more of the childcare role while the affected parent assumes other household responsibilities instead.
- Parental education. Less educated parents and those from lower socioeconomic strata will require more one-to-one training rather than group-based training in BPT and may not respond quite as well even then.
Side Effects of BPT
When treatments are powerful enough to produce behavior change, it should be no surprise that they can have side effects. Yet even though warnings about their occurrence have been sounded for decades, they have received little notice in clinical practice. It is important, therefore, to be aware of the following sorts of adverse events, common to many psychosocial interventions, among others:
- May increase patient and family distress
- Can increase stigma or fear of stigma in children and teens
- Family or couples’ sessions may increase conflict with others
- Can increase patient anxiety, dissociative episodes, re-experiencing of traumatic events, distorted thinking, etc.
- BPT and behavioral family therapy may increase aggression and family conflict
- Group training of children and teens can lead to deviancy training
- May cause a worsening of disorder symptoms or deterioration in treatment targets
- Can delay getting more effective treatment (i.e., medications)
- May be more expensive than other therapies (medications)
- Often are not monitored or detected by treating clinicians who fail to consider the potential to produce harm
- Less likely to be reported to clinician by patient due to perception it may adversely impact relationship
These and other adverse events (AEs) can occur during BPT (see Barkley, 2018, and Allan & Chacko, 2018, in References). Why? Some of these AEs arise due to variability in children’s psychological characteristics, comorbidity, etc., as well in parental fidelity in implementing the methods. Other AEs may arise from lack of clinician training in implementing these methods. About 10%–24% of parents may report a deterioration in the intended targets of treatment, such as a worsening of their child’s ODD symptoms or other conduct problems and of parent-child/teen conflict as a function of BPT. Some of these cases had quite severe ODD (or possibly DMDD) symptoms. Thus, instituting limit setting, discipline, or even contingent use of privileges was enough to spark greater conflict between parents and children or even an escalation to violence by the child. Other children may experience an increase in sadness or depression and decrease in self-worth especially during the use of disciplinary methods.
Care therefore needs to be taken to ask about such adverse events periodically during training and not just naively assume that there is never any worsening of parent-child relations from such programs. And perhaps if the child or teen is already noted to be physically violent, then alternative programs probably need to be used, such as that by Greene on collaborative problem solving. Or clinicians can at least implement only the positive reinforcement aspects of the BPT program.
Summary
This
course has described the nature of oppositional defiant behavior and stressed
the importance of focusing on it as the major target of any parent training
program. The processes whereby children may develop, maintain, or increase
their rate of oppositional, defiant, or noncompliant behavior were discussed in
some detail, and it appears that such behavior is partly if not chiefly
sustained by its success at family coercion – terminating parental demands and
enabling the child to escape or avoid generally unpleasant, effortful, or boring
tasks assigned by parents, while permitting the child to continue in a
previous, more desirable activity. It was shown that parents may also come to
escalate their own negative behavior toward the child because such behavior
occasionally succeeds at terminating ongoing unpleasant child behavior, such as
tantrums or defiance, and getting eventual child compliance. Both parents and
children may be more predisposed toward such types of coercive behavior by
virtue of their particular profile of temperamental patterns and psychological
disorders. Larger contextual events such as stress, marital discord, parental
social isolation, or events impacting the family from outside may serve to
increase the probability of defiant child behavior by virtue of the toll these
events take on the consistency of parental management of the child, the
positive reinforcement of compliant child behavior, and the general monitoring
of child activities by parents.
Specific instructions for how to implement the steps of the
author’s parent training program can be found in the text, Defiant Children (Barkley, 2013). Assessment tools are provided
in the book for clinicians to use in their treatment to monitor behavior of
parents and assess progress. The manual also includes step-by-step
instructions to clinicians on how to implement each step as well as parent
handouts on the methods they have been instructed to use at each step.
Other
parent training programs having some overlap with the author’s program would
include Parent-Child Interaction Therapy by Shelia Eyberg, The Incredible Years
by Carolyn Webster-Stratton, The Noncompliant Child by Robert McMahon and Rex
Forehand, The Community Opportunities for Parent Education (COPE) program by
Charles Cunningham, and the Triple P Positive Parenting Program by Matthew
Sanders, among others. These are reasonable and scientifically validated
alternatives. More about them can be found on the Internet at major online
booksellers and by using Google Scholar as a search engine to explore scientific
journal publications about them.
References
Abidin,
R. R. (1995). The Parenting Stress Index (3rd ed.). Lutz, FL:
Psychological Assessment Resources.
Abikoff,
H., & Hechtman, L. (1995, June). Preliminary results of a multi-modal
treatment program for ADHD children. Paper presented at the annual meeting of
the International Society for Research in Child and Adolescent Psychopathology,
London, England.
Achenbach,
T. M. (2014). Manual for the Child Behavior Checklist – Cross-Informant Version.
Burlington, VT: Thomas Achenbach.
Achenbach,
T. M., McConaughy, S. H., & Howell, C. T. (1987). Child/adolescent
behavioral and emotional problems: Implications of cross-informant correlations
for situational specificity. Psychological Bulletin, 101, 213-232.
Adesso,
V. J., & Lipson, J. W. (1981). Group training of parents as therapists for
their children. Behavior Therapy, 12, 625-633.
Aebi,
M., Muller, U. C., Asherson, P., Banaschewski, T., Buitelaar, J., Ebstein, R.,
Eisenberg, J., Gill, M., Manor, I., Miranda, A., Oades, R. D., Roeyers, H.,
Rothenberger, A., Sergeant, J., Sonuga-Barke, E., Thompson, M., Taylor, E.,
Faraone, S. V., & Steinhausen, H. C. (2010). Predictability of
oppositional defiant disorder and symptom dimensions in children and
adolescents with ADHD combined type. Psychological Medicine, 40, 2089-2100.
Allan, C., & Chacko, A. (2018). Adverse events in behavioral parent training for children with ADHD: An under-appreciated phenomenon. The ADHD Report, 28(1), 4-8.
American
Psychiatric Association. (1987). Diagnostic and statistical manual of mental
disorders (3rd ed., rev.). Washington, DC: Author.
American
Psychiatric Association. (2000). Diagnostic and statistical manual of mental
disorders (4th ed.). Washington, DC: Author.
American
Psychiatric Association. (2013). Diagnostic and statistical manual of mental
disorders (5th ed.). Washington, DC: Author.
Americans
with Disabilities Act of 1990, 42 U.S.C.A. § 12101 et seq. (West 1993).
Anastopoulos,
A. D., Guevremont, D. C., Shelton, T. L., & DuPaul, G. J. (1992). Parenting
stress among families of children with attention deficit hyperactivity
disorder. Journal of Abnormal Child Psychology, 20, 503-520.
Anastopoulos,
A. D., Shelton, T. L., DuPaul, G. J., & Guevremont, D. C. (1993). Parent
training for attention-deficit hyperactivity disorder: Its impact on parent
functioning. Journal of Abnormal Child Psychology, 21, 581-596.
Anderson,
J. C., Williams, S., McGee, R., & Silva, P. A. (1987). DSM-III disorders in
preadolescent children. Archives of General Psychiatry, 44, 69-78.
Angold, A., Costello, E. J.,
& Erkanli, A. (1999). Comorbidity. Journal of Child Psychology and
Psychiatry, 40, 57-88.
Arnold, E. A., Herbert, S. D., & Stowe, R. M. (2015). Parenting hyperactive preschoolers: Clinician guide. New York: Oxford University Press.
Atkeson,
B. M., & Forehand, R. (1978). Parent behavioral training for problem
children: An examination of studies using multiple outcome measures. Journal of
Abnormal Child Psychology, 6, 449-460.
August,
G. J., Realmuto, G. M., Joyce, T., & Hektner, J. M. (1999). Persistence
and desistance of oppositional defiant disorder in a community sample of
children with ADHD. Journal of the American Academy of Child and Adolescent
Psychiatry, 38, 1262-1270.
Barkley,
R. A. (1985). The social interactions of hyperactive children: Developmental
changes, drug effects, and situational variation. In R. McMahon & R. Peters
(Eds.), Childhood disorders: Behavioral-developmental approaches (pp. 218-243).
New York: Brunner/Mazel.
Barkley,
R. A. (1987). Defiant children: A clinician’s manual for parent training. New
York: Guilford Press.
Barkley,
R. A. (2006). Attention-deficit hyperactivity disorder: A handbook for
diagnosis and treatment (3rd ed.). New York: Guilford Press.
Barkley,
R. A. (2010). Deficient emotional self-regulation: a core component of
attention-deficit/hyperactivity disorder. Journal of ADHD and Related
Disorders, 1, 5-37.
Barkley,
R. A. (2011). Barkley Adult ADHD Rating Scale-IV. New York: Guilford Press.
Barkley,
R. A. (2012a). Barkley Functional Impairment Scale - Children and
Adolescents. New York: Guilford Press.
Barkley,
R. A. (2012b). The Executive Functions: What They Are, How They Work, and Why
They Evolved. New York: Guilford Press.
Barkley,
R. A. (2012c). Barkley Deficits in Executive Functioning Scale - Children and
Adolescents. New York: Guilford Press.
Barkley,
R. A. (2013). Defiant children: A clinician’s manual for parent training (3rd
ed.). New York: Guilford Press.
Barkley, R. A. (2018a). Focus on the side effects of psychosocial treatments for children and teens with ADHD: A special issue. The ADHD Report, 26(1), 1-4.
Barkley, R. A. (2018b). Adverse events associated with behavior management training for families experiencing parent-ADHD teen conflict. The ADHD Report, 26(2), 1-6.
Barkley, R. A. (2022). Treating ADHD in Children and Adolescents: What Every Clinician Needs to Know. New York: Guilford Press.
Barkley,
R. A., Anastopoulos, A. D., Guevremont, D. G., & Fletcher, K. F. (1992).
Adolescents with attention deficit hyperactivity disorder: Mother-adolescent
interactions, family beliefs and conflicts, and maternal psychopathology. Journal
of Abnormal Child Psychology, 20, 263-288.
Barkley,
R. A. & Benton, C. (2013). Your Defiant Child: 8 Steps to Better Behavior
(2nd ed.). New York: Guilford Press.
Barkley,
R. A., Edwards, G., & Robin, A. R. (1999). Defiant Teens: A Clinician’s
Manual for Assessment and Family Intervention. New York: Guilford Press.
Barkley, R. A., Edwards, G.,
Laneri, M., Fletcher, K., & Metevia, L. (2001b). The efficacy of
problem-solving communication training alone, behavior management training
alone, and their combination for parent-adolescent conflict in teenagers with
ADHD and ODD. Journal of Consulting and Clinical Psychology, 69, 926-941.
Barkley, R. A. &
Fischer, M. (2011). Predicting impairment in major life activities and
occupational functioning in hyperactive children as adults: Self-reported
executive function (EF) deficits vs. EF tests. Developmental Neuropsychology,
36(2), 137-161.
Barkley,
R. A., Fischer, M., Edelbrock, C. S., & Smallish, L. (1990). The adolescent
outcome of hyperactive children diagnosed by research criteria: I. An 8-year
prospective follow-up study. Journal of the American Academy of Child and
Adolescent Psychiatry, 29, 546-557.
Barkley,
R. A., Fischer, M., Edelbrock, C. S., & Smallish, L. (1991). The adolescent
outcome of hyperactive children diagnosed by research criteria: III.
Mother-child interactions, family conflicts, and maternal psychopathology. Journal
of Child Psychology and Psychiatry, 32, 233-256.
Barkley,
R. A., Guevremont, D. G., Anastopoulos, A. D., & Fletcher, K. (1992). A
comparison of three family therapy programs for treating family conflicts in
adolescents with attention-deficit hyperactivity disorder. Journal of
Consulting and Clinical Psychology, 60, 450-462.
Barkley,
R. A., & Murphy, K. R. (2006). Attention Deficit Hyperactivity Disorder: A
Clinical Workbook (2nd ed.). New York: Guilford Press.
Barkley, R. A. & Murphy, K. R. (2011). The nature of
executive function (EF) deficits in daily life activities in adults with ADHD
and their relationship to performance on EF tests. Journal of Psychopathology
and Behavioral Assessment. 33, 137-158.
Barkley, R. A., Murphy, K. R.,
& Fischer, M. (2008). DHD in Adults: What the Science Says. New York:
Guilford Press.
Barkley, R. A., Shelton, T. L.,
Crosswait, C., Moorehouse, M., Fletcher, K., Barrett, S., Jenkins, L., &
Metevia, L. (2000). Multi-method psycho-educational intervention for preschool
children with disruptive behavior: preliminary results at post-treatment. Journal of Child Psychology and Psychiatry, 41, 319-332.
Barth, R. (1979). Home-based
reinforcement of school behavior: A review and analysis. Review of Educational Research, 49, 436-458.
Bean, A. W., & Roberts, M. W.
(1981). The effects of time-out release contingencies on changes in child
noncompliance. Journal of Abnormal Child Psychology, 9, 95-105.
Beauchaine, T. P., Hinshaw, S.
P., & Pang, K. L. (2010). Comorbidity of attention-deficit/hyperactivity
disorder and early-onset conduct disorder: biological, environmental, and
developmental mechanisms. Clinical Psychology: Science and Practice, 17,
Beck, A. T., Steer, R. A., &
Garbin, M. G. (1988). Psychometric properties of the Beck Depression Inventory:
Twenty-five years of evaluation. Clinical Psychology Review, 8, 77-100.
Becker, W. (1971). Parents are teachers. Champaign-Urbana, IL: Research Press.
Bell, R. Q., & Harper, L. V.
(1977). Child effects on adults. Hillsdale, NJ: Erlbaum.
Belsky, J., Fearon, R. M. P.,
& Bell, B. (2007). Parenting, attention and externalizing problems:
testing mediation longitudinally, repeatedly and reciprocally. Journal of
Child Psychology and Psychiatry, 48, 1233-1242.
Bernal, M. E., Klinnert, M. D.,
& Schultz, L. A. (1980). Outcome evaluation of behavioral parent training
and client-centered parent counseling for children with conduct problems. Journal
of Applied Behavior Analysis, 13, 677-691.
Biederman, J., Faraone, S. V.,
Keenan, K., & Tsuang, M. T. (1991). Evidence of a familial association
between attention deficit disorder and major affective disorders. Archives of
General Psychiatry, 48, 633-642.
Biederman, J., Faraone, S. V.,
Millberger, S., Curtis, S., Chen, L., Marrs, A., Ouellette, C., Moore, P.,
& Spencer, T. (1996). Predictors of persistence and remission of ADHD into
adolescence: Results from a four-year prospective follow-up study. Journal of
the American Academy of Child and Adolescent Psychiatry, 35, 343-351.
Biederman, J., Petty, C. R.,
Dolan, C., Hughes, S., Mick, E., Monuteaux, M. C., & Faraone, S. V. (2008).
The long-term longitudinal course of oppositional defiant disorder and conduct
disorder in ADHD boys: findings from a controlled 10-year prospective
longitudinal follow-up. Psychological Medicine, 38, 1027-1036.
Biederman, J., Petty, C. R.,
Monuteaux, M. C., Mick, E., Parcell, T., Westerberg, D., & Faraone, S. V.
(2008). The longitudinal course of comorbid oppositional defiant disorder in
girls with attention-deficit/hyperactivity disorder: Findings from a controlled
5-year prospective longitudinal follow-up study. Journal of Developmental and
Behavioral Pediatrics, 29, 501-507.
Blouin, B., Maddeaux, C.,
Fireston, J. S., & Stralen, J. van (2010). Predicting response of ADHD
symptoms to methylphenidate treatment based on comorbid anxiety. Journal of Attention
Disorders, 13, 414-419.
Blum, N. J., Williams, G. E.,
Friman, P. C., & Christophersen, E. R. (1995). Disciplining young children:
The role of verbal instructions and reasoning. Pediatrics, 96, 336-341.
Bonham, M. D., Stanley, D. C., Waters, A. M., & Elvin, O. M. (2021). Inhibitory control deficits in children with oppositional defiant disorder and conduct disorder compared to attention deficit/hyperactivity disorder: A systematic review. Research on Child and Adolescent Psychopathology, 49, 39-62.
Booker, J. A., Capriola-Hall, Dunsmore, J. C., Greene, R. W., & Ollendick, T. H. (2018). Change in maternal stress for families in treatment for their children with oppositional defiant disorder. Journal of Child and Family Studies, 27, 2552-2561.
Booker, J. A., Capriola-Hall, Greene, R. W., & Ollendick, T. H. (2020). The parent-child relationship and posttreatment child outcomes across two treatments for oppositional defiant disorder. Journal of Clinical Child and Adolescent Psychology, 49, 405-419.
Breen, M. J., & Barkley, R.
A. (1988). Child psychopathology and parenting stress in girls and boys having
attention deficit disorder with hyperactivity. Journal of Pediatric Psychology,
13, 265-280.
Burke, J. D., Evans, S. C., & Carlson, G. A. (2022). Debate: Oppositional defiant disorder is a real disorder. Child and Adolescent Mental health, 27(3), 297-299.
Burke, J. D., Hipwell, A. E.,
& Loeber, R. (2010). Dimensions of oppositional defiant disorder as predictors
of depression and conduct disorder in preadolescent girls. Journal of the
American Academy of Child and Adolescent Psychiatry, 49, 484-492.
Burke, J. D., Johnston, O. G., & Butler, E. J. (2021). The irritable and oppositional dimensions of oppositional defiant disorder: Integral factors in the explanation of affective and behavioral psychopathology. Child and Adolescent Psychiatry Clinics. Epub ahead of print.
Burke, J. D., & Loeber, R.
(2010). Oppositional defiant disorder and the explanation of the comorbidity
between behavioral disorders and depression. Clinical Psychology: Science and
Practice, 17, 319-326
Burke, J. D., & Romano-Verthelyi, A. M. (2018). Oppositional Defiant Disorder. In M. Martel (Ed.). Developmental Pathways to Disruptive, Impulse-Control and Conduct Disorders (pp. 21-52). New York: Academic Press.
Burke, J. D., Waldman, I., &
Lahey, B. B. (2010). Predictive validity of childhood oppositional defiant
disorder and conduct disorder: Implications for the DSM-V. Journal of Abnormal
Psychology, 119, 739-751.
Burns, C. L. & Walsh, J. A.
(2002). The influence of ADHD-hyperactivity/impulsivity symptoms on the
development of oppositional defiant symptoms in a 2-year longitudinal study.
Journal of Abnormal Child Psychology, 30, 245-256.
Calvert, S. C., & McMahon, R.
J. (1987). The treatment acceptability of a behavioral parent training program
and its components. Behavior Therapy, 2, 165-179.
Capaldi, D. M. (1992).
Co-occurrence of conduct problems and depressive symptoms in early adolescent
boys: II. A 2-year follow-up at grade 8. Development and Psychopathology, 4,
125-144.
Carlson, G. A., & Meyer, S.
E. (2006). Phenomenology and diagnosis of bipolar disorder in children,
adolescents, and adults: complexities and developmental issues. Development
and Psychopathology, 18, 939-969.
Chacko, A., Allan, C. C., Uderman, J., Cornwell, M., Anderson, L., & Chimiklis, A. (2015). Training parents of youth with ADHD. In R. A. Barkley (Ed.). Attention deficit hyperactivity disorder: A handbook for diagnosis and treatment (4th. ed.)(pp. 513-536). New York: Guilford Publications.
Chacko, A., Wymbs, B.T., Chimiklis, A., Wymbs, F.A., & Pelham, W.E. (2012). Evaluating a comprehensive strategy to improve engagement to group-based behavioral parent training for high-risk families of children with ADHD. Journal of Abnormal Child Psychology, 40, 1351-1362.
Chacko, A., Wymbs, B. T.,
Flammer-Rivera, L. M., Pelham, W. E. Walker, K. S., Arnold, F. W.,
Visweswaraiah, H., Swanger-Gagne, M. Girio, E. L., Pirvics, L. L., &
Herbst, L. (2008). A pilot study of the feasibility and efficacy of the
strategies to enhance positive parenting (STEPP) program for single mothers of
children with ADHD. Journal of Attention Disorders, 12, 270-280.
Chacko, A., Wymbs, B. T., Wymbs,
F. A., Pelham, W. E. Jr., Swanger-Gagne, M. S., Girio, E., Pirvics, L., Herbst,
L. Guzzo, J., Phillips, C., & O’Connor, B. (2009). Enhancing traditional parent
training for single mothers of children with ADHD. Journal of Clinical Child
and Adolescent Psychology, 38, 206-213.
Chen, H., Lin, X., Heath, M. A., & Ding, W. (2020). Family violence and oppositional defiant disorder symptoms: The role of parental alienation and child emotion regulation. Child 7 Family Social Work, 25(4), 964-972.
Chen, M., & Johnston, C.
(2007). Maternal inattention and impulsivity and parenting behaviors. Journal
of Clinical Child and Adolescent Psychology, 36, 455-468.
Chen, M., & Johnston, C.
(2012). Interparent childrearing disagreement, but not dissimilarity, predicts
child problems after controlling for parenting effectiveness. Journal of
Clinical Child and Adolescent Psychology, 41, 189-201.
Christensen, A., Johnson, S. M.,
Phillips, S., & Glasgow, R. E. (1980). Cost effectiveness of behavioral
family therapy. Behavior Therapy, 11, 208-226.
Christophersen, E. R., Barnard,
S. R., & Barnard, J. D. (1981). The family training program manual: The
home chip system. In R. A. Barkley, Hyperactive children: A handbook for
diagnosis and treatment (pp. 437-448). New York: Guilford Press.
Chronis, A. M., Chacko, A.,
Fabiano, G. A., Wymbs, B. T., & Pelham, W. E. Jr. (2004). Enhancements to
the behavioral parent training paradigm for families of children with ADHD:
Review and future directions. Clinical Child and Family Psychology Review, 7,
1-27.
Chronis, A. M., Lahey, B. B.,
Pelham, W. E. Jr., Williams, S. H., Baumann, B. L., Kipp, H., Jones, H. A.,
& Rathouz, P. J. (2007). Maternal depression and early positive parenting
predict future conduct problems in young children with
attention-deficit/hyperactivity disorder. Developmental Psychology, 43, 70-82.
Chronis-Tuscano, A., O’Brien, K.
A., Johnston, C., Jones, H. A., Clarke, T. L., Raggi, V. L., Rooney, M. E.,
Diaz, Y., Pian, J., & Seymour, K. E. (2011). The relation between maternal
ADHD symptoms & improvement in child behavior following brief behavioral
parent training is mediated by change in negative parenting. Journal of
Abnormal Child Psychology, 39, 1047-1057.
Chronis-Tuscano, A., Raggi, V.
L., Clarke, T. L., Rooney, M. E., Diaz, Y., & Pian, J. (2008).
Associations between maternal attention-deficit/hyperactivity disorder symptoms
and parenting. Journal of Abnormal Child Psychology. 36, 1237-1250.
Chronis-Tuscano, A., Seymour, K.
E., Stein, M. A., Jones, H. A., Jiles, C. D., Rooney, M. E., Conlon, C. J.,
Efron, L. A., Wagner, S. A., Pian, J., & Robb, A. S. (2008). Efficacy of
osmotic-release oral system (OROS) methylphenidate for mothers with
attention-deficit/hyperactivity disorder (ADHD): preliminary report of effects
on ADHD symptoms and parenting. Journal of Clinical Psychiatry, 69, 1-10.
Conner, D. F. (2006).
Stimulants. In R. A. Barkley (Ed.), Attention deficit hyperactivity disorder:
a handbook for diagnosis and treatment (3rd ed.) (pp. 608-647). New
York: Guilford Press.
Connor, D. F., Steeber, J., &
McBurnett, K. (2010). A review of attention-deficit/hyperactivity disorder
complicated by symptoms of oppositional defiant disorder or conduct disorder.
Journal of Developmental and Behavioral Pediatrics, 31, 427-440.
Copeland, W. E., Miller-Johnson,
S., Keeler, G., Angold, A., & Costello, E. J. (2007). Childhood
psychiatric disorders and young adult crime: a prospective, population-based
study. American Journal of Psychiatry, 164, 1668-1675.
Crits-Cristoph, P., & Mintz,
J. (1991). Implications of therapist effects for the design and analysis of
comparative studies of psychotherapies. Journal of Consulting and Clinical
Psychology, 59, 20-26.
Cunningham, C. E., Bremner, R.,
& Boyle, M. (1995). Large group community-based parenting programs for
families of preschoolers at risk for disruptive behavior disorders:
Utilization, cost effectiveness, and outcome. Journal of Child Psychology and
Psychiatry, 36, 1141-1159.
Cunningham, C. E., Bremner, R., & Secord, M. (2006). COPE: The Community Parent Education Program: A School-Based Family Systems Oriented Workshop for Parents of Children with Disruptive Behavior Disorders. Hamilton, Ontario: COPE Works.
Cunningham, C. E., & Boyle,
M. H. (2002). Preschoolers at risk for attention-deficit hyperactivity
disorder and oppositional defiant disorder: family, parenting, and behavioral
correlates. Journal of Abnormal Child Psychology, 30, 555-569.
Curtis, D. F. (2010). ADHD
symptom severity following participation in a pilot, 10-week, manualized
family-based behavioral intervention. Child and Family Behavior Therapy, 32,
231-241.
Dachew, B. A., Scott, J. G., & Heron, J. E. (2021). Association of maternal depressive symptoms during the perinatal period with oppositional defiant disorder in children and adolescents. JAMA Network Open. Epub ahead of print.
Dadds, M. R., & McHugh, T. A.
(1992). Social support and treatment outcome in behavioral family therapy for
child conduct problems. Journal of Consulting and Clinical Psychology, 60,
252-259.
Dadds, M. R., Schwartz, S., &
Sanders, M. R. (1987). Marital discord and treatment outcome in behavioral
treatment of child conduct disorders. Journal of Consulting and Clinical
Psychology, 55, 396-403.
Danforth, J. S., Barkley, R. A.,
& Stokes, T. F. (1991). Observations of parent-child interactions with
hyperactive children: Research and clinical implications. Clinical Psychology
Review, 11, 703-727.
Danforth, J. S., Harvey, E.,
Ulaszek, W. R., & McKee, T. E. (2006). The outcome of group parent
training for families of children with attention-deficit hyperactivity disorder
and defiant/aggressive behavior. Journal of Behavior Therapy and Experimental
Psychiatry, 37, 188-205.
Day, D. E., & Roberts, M. W.
(1982). An analysis of the physical punishment component of a parent training
program. Journal of Abnormal Child Psychology, 11, 141-152.
Deault, L. C. (2010). A
systematic review of parenting in relation to the development of comorbidities
and functional impairments in children with attention-deficit/hyperactivity
disorder (ADHD). Child Psychiatry and Human Development, 41, 168-192.
Derogatis, L. (1994). Manual for the Symptom Checklist 90 – Revised (SCL-90-R). Indianapolis, IN: Pearson Assessments.
Dishion, T. J., & Patterson,
G. R. (1992). Age effects in parent training outcome. Behavior Therapy, 23,
719-729.
Dodge, K. A., McClaskey, C. L.,
& Feldman, E. (1985). A situational approach to the assessment of social
competence in children. Journal of Consulting and Clinical Psychology, 53,
344-353.
D’Onofrio, B. M., Goodnight, J.
A., Van Hulle, C. A., Rodgers, J. L., Rathouz, P. J., Waldman, I. D., &
Lahey, B. B. (2009). Maternal age at childbirth and offspring disruptive
behaviors: testing the causal hypothesis. Journal of Child Psychology and
Psychiatry, 50, 1018-1028.
Dougherty, E. H. & Dougherty,
A. (1977). The daily report card: a simplified and flexible package for
classroom behavior management. Psychology in the Schools, 14, 191-195.
Drabick, D. A. G., & Gadow,
K. D. (2012). Deconstructing oppositional defiant disorder: clinic-based
evidence for an anger/irritability phenotype. Journal of the American Academy
of Child and Adolescent Psychiatry, 51, 384-393.
Drugli, M. B., Larsson, B.,
Fossum, S., Morch, W. T. (2010). Five- to six-year outcome and its prediction
for children with ODD/CD treated with parent training. Journal of Child
Psychology and Psychiatry, 51, 559-566.
Dubey, D. R., O’Leary, S. G.,
& Kaufman, K. F. (1983). Training parents of hyperactive children in child
management: A comparative outcome study. Journal of Abnormal Child Psychology, 11,
229-246.
Dumas, J. E. (1984).
Interactional correlates of treatment outcome in behavioral parent training. Journal
of Consulting and Clinical Psychology, 52, 946-954.
Dumas, J. E., Gibson, J. A.,
& Albin, J. B. (1989). Behavioral correlates of maternal depressive
symptomatology in conduct disordered children. Journal of Consulting and
Clinical Psychology, 57, 516-521.
Dumas, J. E., & Wahler, R. G.
(1983). Predictors of treatment outcome in parent training: Mother insularity
and socioeconomic disadvantage. Behavioral Assessment, 5, 301-313.
Dumas, J. E., & Wahler, R. G.
(1985). Indiscriminate mothering as a contextual factor in
aggressive-oppositional child behavior: "Damned if you do and damned if you don't." Journal of Abnormal Child Psychology, 13, 1-17.
DuPaul, G. J., Anastopoulos, A.
D., Power, T. J., Reid, R., Ikeda, M. J., & McGoey, K. E. (1998). ADHD
Rating Scale - IV. New York: Guilford Press
DuPaul, G. J., & Stoner, G.
(2003). ADHD in the schools: Assessment and intervention strategies (2nd ed.). New York: Guilford Press.
Dyer, W. (1991). Your erroneous
zones. New York: William Morrow.
Elgar, F. J., Mills, R. S. L.,
McGrath, P. J., Waschbusch, D. A., Brownridge, D. A. (2007). Maternal and
paternal depressive symptoms and child maladjustment: the mediating role of
parental behavior. Journal of Abnormal Child Psychology, 35, 943-955.
Ellis, A., & Dryden, W.
(2007). The practice of rational emotive behavior therapy (2nd ed.).
New York: Springer.
Ellis, A., & Harper, R. A.
(1977). A guide to rational living. New York: Wilshire.
Ellis, B., & Nigg, J. (2009).
Parenting practices and attention-deficit/hyperactivity disorder: new findings
suggest partial specificity of effects. Journal of the American Academy of
Child and Adolescent Psychiatry, 48,148-154.
Evans, S. W., Vallano, M. D.,
& Pelham, W. (1994). Treatment of parenting behavior with a
psychostimulant: A case study of an adult with attention-deficit hyperactivity
disorder. Journal of Child and Adolescent Psychopharmacology, 4, 63-69.
Eyberg, S. M., & Matarazzo R.
G. (1980). Training parents as therapists: A comparison between individual
parent-child interaction training and parent group didactic training. Journal
of Clinical Psychology, 36, 492-499.
Eyberg, S. M., Nelson, M. N.,
& Boggs, S. R. (2008). Evidence-based psychosocial treatments for children
and adolescents with disruptive behavior. Journal of Clinical Child and
Adolescent Psychology, 37, 215-237.
Eyberg, S. M., & Robinson, E.
A. (1982). Parent-child interaction training: Effects on family functioning. Journal
of Clinical Child Psychology, 11, 130-137.
Fabiano, G. A., Vujnovic, R. K.,
Pelham, W. E., Waschbusch, D. A., Massetti, G. M., Pariseau, M. E., Naylor, J.,
Yu, J., Robins, M., Cronefix, T., Greiner, A. R., & Volker, M. (2010).
Enhancing the effectiveness of special education programming for children with
attention deficit hyperactivity disorder using a daily report card. School
Psychology Review, 39, 219-239.
Faraone, S. V., Biederman, J.,
Lehman, B., Keenan, K., Norman, D., Seidman, L. J., Kolodny, R., Kraus, I.,
Perrin, J., & Chen, W. (1993). Evidence for the independent familial
transmission of attention deficit hyperactivity disorder and learning
disabilities: Results from a family genetic study. American Journal of
Psychiatry, 150, 891-895.
Farrington, D. P. (1995). The
twelfth Jack Tizard memorial lecture. The development of offending and
antisocial behavior from childhood: Key findings from the Cambridge study in
delinquent development. Journal of Child Psychology and Psychiatry, 360,
929-964.
Fergusson, D. M., Horwood, L. J.,
& Lynskey, M. T. (1993). Prevalence and comorbidity of DSM-III-R diagnoses
in a birth cohort of 15-year-olds. Journal of the American Academy of Child and
Adolescent Psychiatry, 32, 1127-1133.
Fernandez, M. A., & Eyberg,
S. M. (2009). Predicting treatment and follow-up attrition in Parent-Child
Interaction Therapy. Journal of Abnormal Child Psychology, 37, 431-441.
Firestone, P., Kelly, M., &
Fike, S. (1980). Are fathers necessary in parent training groups? Journal of
Clinical Child Psychology, 44-47.
Firestone, P., Kelly, M. J.,
Goodman, J. T., & Davey, J. (1981). Differential effects of parent training
and stimulant medication with hyperactives. Journal of the American Academy of
Child Psychiatry, 20, 135-147.
Firestone, P., & Witt, J. E.
(1982). Characteristics of families completing and prematurely discontinuing a
behavioral parent training program. Journal of Pediatric Psychology, 7,
209-222.
Fischer, M. (1990). Parenting
stress and the child with attention deficit hyperactivity disorder. Journal of
Clinical Child Psychology, 19, 337-346.
Fischer, M., Barkley, R. A.,
Fletcher, K., & Smallish, L. (1993). The stability of dimensions of
behavior in ADHD and normal children over an 8-year period. Journal of Abnormal
Child Psychology, 21, 315-337.
Fletcher, K., Fischer, M.,
Barkley, R. A., & Smallish, L. (1996). Sequential analysis of
mother-adolescent interactions of ADHD, ADHD/ODD, and normal teenagers during
neutral and conflict discussions. Journal of Abnormal Child Psychology, 24,
271-297.
Forehand, R., & Scarboro, M.
E. (1975). An analysis of children’s oppositional behavior. Journal of Abnormal
Child Psychology, 3, 27-31.
Forgatch, M., & Patterson, G.
R. (1990). Parents and adolescents living together. Eugene, OR: Castalia.
Frankel, F., & Simmons, J.
Q., III. (1992). Parent behavioral training: Why and when some parents drop
out. Journal of Clinical Child Psychology, 21, 322-330.
Frick, P. J., Lahey, B. B.,
Loeber, R., Stouthamer-Loeber, M., Christ, M. A., & Hanson, K. (1992).
Familial risk factors to oppositional defiant disorder and conduct disorder:
Parental psychopathology and maternal parenting. Journal of Consulting and
Clinical Psychology, 60, 49-55.
Frick, P. J., Van Horn, Y.,
Lahey, B. B., Christ, M. A. G., Loeber, R., Hart, E. A., Tannenbaum, L., &
Hanson, K. (1993). Oppositional defiant disorder and conduct disorder: A
meta-analytic review of factor analyses and cross-validation in a clinic
sample. Clinical Psychology Review, 13, 319-340.
Furlong, M., McGilloway, S., Bywater,
T., Hutchings, J., Smith, S. M., & Donelly, M. (2012). Behavioral and
cognitive-behavioral group-based parenting programmes for early-onset conduct
problems in children aged 3 to 12 (Review). The Chochrane Database of
Systematic Reviews, 2, 1-344.
Gadow, K. D., & Drabick, D.
A. G. (2012). Symptoms of autism and schizophrenia spectrum disorders in
clinically referred youth with oppositional defiant disorder. Research in
Developmental Disabilities, 33, 1157-1168.
Garfield, S. L., & Bergen, A.
E. (Eds.). (1986). Handbook of psychotherapy and behavior change (3rd ed.). New
York: Wiley.
Gerdes, A. C., Haack, L. M.,
& Schneider, B. W. (2012). Parental functioning in families of children
with ADHD: evidence for behavioral parent training and importance of clinically
meaningful change. Journal of Attention Disorders, 16, 147-156.
Goldstein, A. P., Keller, H.,
& Erne, D. (1985). Changing the abusive parent. Champaign, IL: Research
Press.
Goldstein, L. H., Harvey, E. A.,
& Friedman-Weieneth, J. L. (2007). Examining subtypes of behavior problems
among 3-year-old children, Part III: Investigating differences in parenting
practices and parenting stress. Journal of Abnormal Child Psychology, 35,
125-136.
Green, K. D., Forehand, R., &
McMahon, R. J. (1979). Parental manipulation of compliance and noncompliance in
normal and deviant children. Behavior Modification, 3, 245-266.
Greene, R. W., & Ablon, J. S. (2006). Treating explosive kids: The collaborative problem-solving approach. New York: Guilford Publications.
Gresham, F., & Elliott, S.
(1990). Social Skills Rating System. Circle Pines, MN: American Guidance
Service.
Griggs, M. S., & Mikami, A.
Y. (2011). The role of maternal and child ADHD symptoms in shaping
interpersonal relationships. Journal of Abnormal Child Psychology, 39,
437-449.
Haapasalo, J., & Tremblay, R.
E. (1994). Physically aggressive boys from ages 6 to 12: Family background,
parenting behavior, and prediction of delinquency. Journal of Consulting and
Clinical Psychology, 62, 1044-1052.
Harty, S. C., Miller, C. J.,
Newcorn, J. H., & Halperin, J. M. (2009). Adolescents with childhood ADHD
and comorbid disruptive behavior disorders: Aggression, anger, and hostility.
Child Psychiatry and Human Development, 40, 85-97.
Harvey, E. A., Metcalf, L. A.,
Fanton, J. H., & Herbet, S. D. (2011). The role of family experiences and
ADHD in the early development of oppositional defiant disorder. Journal of
Consulting and Clinical Psychology, 79, 784-795.
Harvey, E. A. & Metcalf, L.
A. (2012). The interplay among preschool child and family factors and the
development of ODD symptoms. Journal of Clinical Child and Adolescent
Psychology, 41, 458-470.
Hautmann, C., Eichelberger, I.,
Hanisch, C., Phick, J., Walter, D., & Dopfner, M. (2010). The severely
impaired do profit most: short-term and long-term predictors of therapeutic
change for a parent management training under routine care conditions for
children with externalizing problem behavior. European Child and Adolescent
Psychiatry, 19, 419-430.
Healey, D. M., Gopin, C. B.,
Grossman, B. R., Campbell, S. B., & Halperin, J. M. (2010). Mother-child
dyadic synchrony is associated with better functioning in
hyperactive/inattentive preschool children. Journal of Child Psychology and
Psychiatry, 51, 1058-1066.
Hinshaw, S. P. (1987). On the
distinction between attentional deficits/hyperactivity and conduct
problems/aggression in child psychopathology. Psychological Bulletin, 101,
443-463.
Hinshaw, S. P., Han, S. S.,
Erhardt, D., & Huber, A. (1992). Internalizing and externalizing behavior
problems in preschool children: Correspondence among parent and teacher ratings
and behavior observations. Journal of Clinical Child Psychology, 21, 143-150.
Hinshaw, S. P., & Lee, S. S.
(2012). Conduct and oppositional defiant disorders. In E. J. Mash & R. A.
Barkley (Eds.), Child psychopathology (3rd ed.) (pp. 144-198). New
York: Guilford Press.
Hirshfeld-Becker, D. R., Petty,
C., Micco, J. A., Henin, A., Park, J., Beilin, A., Rosenbaum, J. F., &
Biederman, J. (2008). Disruptive behavior disorders in offspring of parents
with major depression: associations with parental behavior disorders. Journal
of Affective Disorders, 111, 176-184.
Hoffenaar, P. J., & Hoeksma,
J. B. (2002). The structure of oppositionality: response dispositions and
situational aspects. Journal of Child Psychology and Psychiatry, 43, 375-385.
Holden, G. W., Lavigne, V. V.,
& Cameron, A. M. (1990). Probing the continuum of effectiveness in parent
training: Characteristics of parents and preschoolers. Journal of Clinical
Child Psychology, 19, 2-8.
Hoofdakker van den, B. J.,
Veen-Mulders van den, L., Sytema, S., Emmelkam, P. M. G., Minderaa, R. B.,
& Nauta, M. H. (2007). Effectiveness of behavioral parent training for
children with ADHD in routine clinical practice: a randomized controlled
study. Journal of the American Academy of Child and Adolescent Psychiatry, 48,
1263-1271.
Horn, W. F., Ialongo, N.,
Greenberg, G., Packard, T., & Smith-Winberry, C. (1990). Additive effects
of behavioral parent training and self-control therapy with attention deficit
hyperactivity disordered children. Journal of Clinical Child Psychology, 19,
98-110.
Horn, W. F., Ialongo, N. S.,
Pascoe, J. M., Greenberg, G., Packard, T., Lopez, M., Wagner, A., &
Puttler, L. (1991). Additive effects of psychostimulants, parent training, and
self-control therapy with ADHD children. Journal of the American Academy of
Child and Adolescent Psychiatry, 30, 233-240.
Horn, W. F., Iolongo, N.,
Popovich, S., & Peradotto, D. (1987). Behavioral parent training and
cognitive-behavioral self-control therapy with ADD-H children: Comparative and
combined effects. Journal of Clinical Child Psychology, 16, 57-68.
Horton, L. (1984). The father’s
role in behavioral parent training: A review. Journal of Clinical Child
Psychology, 13, 274-279.
Humphreys, L., Forehand, R.,
McMahon, R., & Roberts, M. (1978). Parent behavioral training to modify
child noncompliance: Effects on untreated siblings. Journal of Behavior Therapy
and Experimental Psychiatry, 9, 1-5.
Humphreys, K. L., Aguirre, V. P.,
& Lee, S. S. (2012). Association of anxiety and ODD/CD in children with
and without ADHD. Journal of Clinical Child and Adolescent Psychology, online
first, DOI: 10.1080/15374416.2012.656557.
Humphreys, K. L. & Lee, S. S.
(2011). Risk taking and sensitivity to punishment in children with ADHD, ODD,
ADHD+ODD, and controls. Journal of Psychopathology and Behavioral Assessment,
33, 299-307.
Individuals with Disabilities in
Education Act of 1974, 20 U.S.C.A. § 1400 et seq., reauthorization, 1991.
Jensen, P. S., Watanabe, H. K.,
Richters, J. E., Cortes, R., Roper, M., & Liu, S. (1995). Prevalence of
mental disorder in military children and adolescents: Findings from a two-stage
community survey. Journal of the American Academy of Child and Adolescent
Psychiatry, 34, 1514-1524.
Johnson, S. M., Wahl, G., Martin,
S., & Johansson, S. (1973). How deviant is the normal child? A behavioral
analysis of the preschool child and his family. In R. D. Rubin, J. P. Brady,
& J. D. Henderson (Eds.), Advances in behavior therapy (Vol. 4). New York:
Academic Press.
Johnston, C. (1992, February). The
influence of behavioral parent training on inattentive overactive and
aggressive-defiant behaviors in ADHD children. Paper presented at the annual
meeting of the Society for Research in Child and Adolescent Psychopathology,
Johnston, C. (1996). Parent
characteristics and parent-child interactions in families of nonproblem
children and ADHD children with higher and lower levels of oppositional-defiant
behavior. Journal of Abnormal Child Psychology, 24, 85-104.
Johnston, C., Hommersen, P.,
& Seipp, C. M. (2009). Maternal attributions and child oppositional behavior: a longitudinal study of boys with and without attention-deficit/hyperactivity disorder. Journal of Consulting and Clinical Psychology, 77, 189-195.
Johnston, C. & Mash, E. J.,
(2001). Families of children with attention-deficit/hyperactivity disorder:
Review and recommendations for future research. Clinical Child and Family
Psychology Review, 4, 183-207.
Johnston, C., Mash, E. J.,
Miller, N., & Ninowski, J. E. (2012). Parenting in adults with attention-deficit/hyperactivity
disorder (ADHD). Clinical Psychology Review, 32, 215-228.
Johnston, C. & Ohan, J. L.
(2005). The importance of parental attributions in families of children with
attention-deficit/hyperactivity and disruptive behavior disorders. Clinical
Child and Family Psychology Review, 8, 167-182.
Jones, H. A., Epstein, J. N.,
Hinshaw, S. P., Owens, E. B., Chi, T. C., Arnold, L. E., Hoza, B., & Wells,
K. C. (2010). Ethnicity as a moderator of treatment effects on parent child
interaction for children with ADHD. Journal of Attention Disorders, 13,
592-600.
Joyner, K. B., Silver, C. H.,
& Stavinoha, P. L. (2009). Relationship between parenting stress and
ratings of executive functioning in children with ADHD. Journal of
Psychoeducational Assessment, 27, 452-464.
Jurbergs, N., Palcic, J. L.,
& Kelley, M. L. (2008). School-home notes with and without response cost:
increasing attention and academic performance in low-income children with
attention-deficit/hyperactivity disorder. School Psychology Quarterly, 22,
358-379.
Jurbergs, N., Palcic, J. L.,
& Kelley, M. L. (2010). Daily behavior report cards with and without
home-based consequences: improving classroom behavior in low income, African
American children with ADHD. Child and Family Behavior Therapy, 32, 177-195.
Kaminski, J. W., Valle, L. A.,
Filene, J. H., & Boyle, C. L. (2008). A meta-analytic review of components
associated with parent training effectiveness. Journal of Abnormal Child
Psychology, 36, 567-589.
Kazdin, A. E. (1980).
Acceptability of time out from reinforcement procedures for disruptive child
behavior. Behavior Therapy, 11, 329-344.
Kazdin, A. E. (1991).
Effectiveness of psychotherapy with children and adolescents. Journal of
Consulting and Clinical Psychology, 58, 729-740.
Keenan, K., & Shaw, D. S.
(1994). The development of aggression in toddlers: A study of low-income
families. Journal of Abnormal Child Psychology, 22, 53-77.
Kelley, M. L., Embry, L. H.,
& Baer, D. M. (1979). Skills for child management and family support. Behavior
Modification, 3, 373-396.
Knapp, P. A., & Deluty, R. H.
(1989). Relative effectiveness of two behavioral parent training programs. Journal
of Clinical Child Psychology, 18, 314-322.
Kolko, D. J., & Pardini, D.
A. (2010). ODD dimensions, ADHD, and callous-unemotional traits as predictors
of treatment response in children with disruptive behavior disorders. Journal
of Abnormal Psychology, 119, 713-725.
Lahey, B. B., Gendrich, J. G.,
Gendrich, S. I., Schnelle, J. F., Gant, D. S., & McNees, M. P. (1977). An
evaluation of daily report cards with minimal teacher and parent contacts as an
efficient method of classroom intervention. Behavior Modification, 1, 381-394.
Lahey, B. B., & Loeber, R.
(1994). Framework for a developmental model of oppositional defiant disorder
and conduct disorder. In D. K. Routh (Ed.), Disruptive behavior disorders in
childhood (pp. 139-180). New York: Plenum Press.
Lahey, B. B., Loeber, R., Quay,
H. C., Frick, P. J., & Grimm, J. (1992). Oppositional defiant and conduct
disorders: Issues to be resolved for DSM-IV. Journal of the American Academy of
Child and Adolescent Psychiatry, 31, 539-546.
Lahey, B. B., Van Hulle, C. A.,
Rathouz, P. J., Rodgers, J. L., D’Onofrio, B. M., & Waldman, I. D. (2009).
Are oppositional-defiant and hyperactive-inattentive symptoms developmental
precursors to conduct problems in late childhood? Genetic and environmental
links. Journal of Abnormal Child Psychology, 37, 45-58.
Lanza, H. I., & Drabick, D.
A. G. (2012). Family routine moderates the relation between child impulsivity
and oppositional defiant disorder symptoms. Journal of Abnormal Child
Psychology, online first, DOI 10.1007/s10802-010-9447-5
Latham, P., & Latham, R.
(1992). ADD and the law. Washington, DC: JKL Communications.
Leckman-Westin, E., Cohen, P. R.,
& Stueve, A. (2009). Maternal depression and mother-child interaction
patterns: association with toddler problems and continuity of effects to late
childhood. Journal of Child Psychology and Psychiatry, 50, 1176-1184.
Lewinsohn, P. M., Hops, H.,
Roberts, R. E., Seeley, J. R., & Andrews, J. A. (1993). Adolescent
psychopathology: I. Prevalence and incidence of depression and other DSM-III-R
disorders in high school students. Journal of Abnormal Psychology, 102,
133-144.
Lier, P. A. C. van, Ende, J. van
der, Koot, H. M., & Verhulst, F. C. (2007). Which better predicts conduct
problems? The relationship of trajectories of conduct problems with ODD and
ADHD symptoms from childhood into adolescence. Journal of Child Psychology and
Psychiatry, 48, 601-608.
Lilienfeld, S. O., & Marino,
L. (1995). Mental disorder as a Roschian concept: A critique of Wakefield’s
“harmful dysfunction” analysis. Journal of Abnormal Psychology, 104, 411-420.
Lifford, K. J., Harold, G. T.,
& Thapar, A. (2008). Parent-child relationships and ADHD symptoms: a
longitudinal analysis. Journal of Abnormal Child Psychology, 36, 285-296.
Lifford, K. J., Harold, G. T.,
& Thapar, A. (2009). Parent-child hostility and child ADHD symptoms: a
genetically sensitive and longitudinal analysis. Journal of Child Psychology
and Psychiatry, 50, 1468-1476.
Little, L. M., & Kelley, M.
L. (1989). The efficacy of response cost procedures for reducing children’s
noncompliance to parental instructions. Behavior Therapy, 20, 515-534.
Locke, H. J., & Wallace, K.
M. (1959). Short marital adjustment and prediction tests: Their reliability and
validity. Journal of Marriage and Family Living, 21, 251-255.
Loeber, R. (1988). Natural
histories of conduct problems, delinquency, and associated substance use. In B.
B. Lahey & A. E. Kazdin (Eds.), Advances in clinical child psychology (Vol.
11, pp. 73-124). New York: Plenum Press.
Loeber, R. (1990). Development
and risk factors of juvenile antisocial behavior and delinquency. Clinical
Psychology Review, 10, 1-41.
Loeber, R., Burke, J., &
Pardini, D. A. (2009). Perspectives on oppositional defiant disorder, conduct
disorder, and psychopathic features. Journal of Child Psychology and
Psychiatry, 50, 133-142.
Loeber, R., Green, S. M., Lahey,
B. B., Christ, M. A. G., & Frick, P. J. (1992). Developmental sequences in
the age of onset of disruptive child behaviors. Journal of Child and Family
Studies, 1, 21-41.
Loeber, R., Green, S., Lahey, B.
B., & Stouthamer-Loeber, M. (1991). Differences and similarities between
children, mothers, and teachers as informants on disruptive behavior disorders.
Journal of Abnormal Child Psychology, 19, 75-95.
Lynskey, M. T., & Fergusson,
D. M. (1994). Childhood conduct problems, attention deficit behaviors, and
adolescent alcohol, tobacco, and illicit drug use. Journal of Abnormal Child
Psychology, 23, 281-302.
Mann, B. J., Borduin, C. M.,
Henggeler, S. W., & Blaske, D. M. (1990). An investigation of systemic
conceptualizations of parent-child coalitions and symptom change. Journal of
Consulting and Clinical Psychology, 3, 336-344.
Mann, B. J., & MacKenzie, E.
P. (1996). Pathways among marital functioning, parental behaviors, and child
behavior problems in school-age boys. Journal of Clinical Child Psychology, 25,
183-191.
Marks, D. J., McKay, K. E.,
Himmelstein, J., Walter, K. J., Newcorn, J. H., & Halperin, J. M. (2000).
Predictors of physical aggression in children with attention-deficit/hyperactivity
disorder. CNS Spectrum, 5, 52-57.
Martin, A., Scahill, L., Charney,
D. S., & Leckman, J. F. (2002). Pediatric psychopharmacology. New York:
Oxford University Press.
Martin, B. (1977). Brief family
intervention: Effectiveness and the importance of including the father. Journal
of Consulting and Clinical Psychology, 45, 1002-1010.
Mash, E. J., & Barkley, R. A.
(Eds.). (2003). Child psychopathology. New York: Guilford Press.
Mash, E. J., & Barkley, R. A.
(Eds.). (2007). Assessment of childhood disorders (3rd ed.). New
York: Guilford Press.
Mash, E. J., & Barkley, R. A.
(Eds.). (2006). Treatment of childhood disorders (3rd ed.). New
York: Guilford Press.
Mash, E. J., & Dozois, D. J.
A. (1996). Child psychopathology: A developmental systems perspective. In E. J.
Mash & R. A. Barkley (Eds.), Child psychopathology (pp. 3-62). New York:
Guilford Press.
Matson, J. L., Rotatori, A. F.,
& Helsel, W. J. (1983). Development of a rating scale to measure social
skills in children: The Matson Evaluation of Social Skills with Youngsters
(MESSY). Behaviour Research and Therapy, 21, 335-340.
Maughan, B., Rowe, R., Messer,
J., Goodman, R., & Meltzer, H. (2004). Conduct disorder and oppositional
defiant disorder n a national sample: developmental epidemiology. Journal of
Child Psychology and Psychiatry, 45, 609-621.
McCart, M. R., Priester, P. E.,
Davies, W. H., & Azen, R. (2006). Differential effectiveness of behavioral
parent-training and cognitive-behavioral therapy for antisocial youth: a
meta-analysis. Journal of Abnormal Child Psychology, 34, 527-543.
McElroy, E. M., & Rodriguez,
C. M. (2008). Mothers of children with externalizing behavior problems:
cognitive risk factors for abuse potential and discipline style and practices.
Child Abuse & Neglect, 32, 774-784.
McGee, R., Feehan, M., Williams,
S., Partridge, F., Silva, P. A., & Kelly, J. (1990). DSM-III disorders in a
large sample of adolescents. Journal of the American Academy of Child and
Adolescent Psychiatry, 29, 611-619.
McMahon, R. J., & Forehand, R.
(1984). Parent training for the noncompliant child. In R. F. Dangel & R. A.
Polster (Eds.), Parent training: Foundations of research and practice (pp.
298-328). New York: Guilford Press.
McMahon, R. J. & Forehand, R.
L. (2005). Helping the noncompliant child: A clinician’s guide to parent
training (2nd ed.). New York: Guilford Press.
McMahon, R. J. & Frick, P. J. (2019). Conduct and oppositional disorders. In M. Prinstein, E. A. Youngstrom, E. J. Mash, & R. A. Barkley (Eds.). Treatment of childhood disorders (Eds.) (pp.102-172). New York: Guilford Publications.
McMahon, R. J., Tiedemann, G. L.,
Forehand, R., & Griest, D. L. (1984). Parental satisfaction with parent
training to modify child noncompliance. Behavior Therapy, 15, 295-303.
Mikolajewski, A. J., & Sheeringa, M. S. (2022). Links between oppositional defiant disorder dimensions, psychophysiology, and interpersonal versus noninterpersonal trauma. Journal of Psychopathology and Behavioral Assessment, 44, 261-275.
Miller, S., Loeber, R., &
Hipwell, A. (2009). Peer deviance, parenting and disruptive behavior among
young girls. Journal of Abnormal Child Psychology, 37, 139-152.
Moffitt, T. E. (1990). Juvenile
delinquency and attention deficit disorder: Boys’ developmental trajectories
from age 3 to age 15. Child Development , 61, 893-910.
Monuteaux, M. C., Faraone, S. V.,
Gross, L. M., & Biederman, J. (2007). Predictors, clinical
characteristics, and outcome of conduct disorder in girls with
attention-deficit/hyperactivity disorder: a longitudinal study. Psychological
Medicine, 37, 1731-1741.
Moshe, K., Karni, A., &
Tirosh, E. (2012). Anxiety and methylphenidate in attention deficit
hyperactivity disorder: a double-blind placebo-drug trial. ADHD Attention
Deficit Hyperactivity Disorder, online first, DOI 10.1007/s12402-012-0078-2.
Moura, M. A. & Burns, G. L.
(2010). Oppositional defiant behavior toward adults and oppositional defiant
behavior toward other children: evidence for two separate constructs with
mothers’ and fathers’ ratings of Brazilian children. Journal of Child
Psychology and Psychiatry, 51, 23-30.
Multimodal Treatment of ADHD
Group. (1999). Moderators and mediators of treatment response for children with
attention-deficit/hyperactivity disorder: the Multimodal Treatment Study of
children with Attention-deficit/hyperactivity disorder. Archives of General
Psychiatry, 56(12), 1088-1096.
Murphy, K. R., & Barkley, R.
A. (1996). Parents of children with attention-deficit/hyperactivity disorder:
Psychological and attentional impairment. American Journal of Orthopsychiatry, 66,
93-102.
Nicholson, J. S., Deboeck, P. R.,
Farris, J. R., Boker, S. M., & Borkowski, J. G. (2011). Maternal
depressive symptomatology and child behavior: transactional relationship with simultaneous bidirectional coupling. Developmental Psychology, 47, 1312-1323.
Nigg, J. T. (2006). What causes
ADHD? New York: Guilford Press.
Nock, M. K., Kazdin, A. E.,
Hiripi, E., & Kessler, R. C. (2007). Lifetime prevalence, correlates, and
persistence of oppositional defiant disorder” results from the National
Comorbidity Survey Replication. Journal of Child Psychology and Psychiatry,
48, 703-713.
Ogden, T., & Hagen, K. A.
(2008). Treatment effectiveness of parent management training in Norway: A
randomized controlled trial of children with conduct problems. Journal of
Consulting and Clinical Psychology, 76, 607-621.
Olson, S. L. (1992). Development
of conduct problems and peer rejection in preschool children: A social systems
analysis. Journal of Abnormal Child Psychology, 20, 327-350.
Olweus, D. (1979). Stability of
aggressive reaction patterns in males: A review. Psychological Bulletin, 86,
852-875.
Olweus, D. (1980). Familial and
temperamental determinants of aggressive behavior in adolescent boys: A causal
analysis. Developmental Psychology, 16, 644-660.
Pardini, D. A., & Fite, P. J.
(2010). Symptoms of conduct disorder, oppositional defiant disorder,
attention-deficit/hyperactivity disorder, and callous-unemotional traits as
unique predictors of psychosocial maladjustment in boys: advancing an evidence
base for DSM-V. Journal of the American Academy of Child and Adolescent
Psychiatry, 49, 1134-1144.
Pardini, D. A., Fite, P. J.,
& Burke, J. D. (2008). Bidirectional associations between parenting
practices and conduct problems in boys from childhood to adolescence: The moderating
effect of age and African-American ethnicity. Journal of Abnormal Child
Psychology, 36, 647-662.
Pardini, D., Obradovic, J., &
Loeber, R. (2006). Interpersonal callousness, hyperactivity/impulsivity,
inattention, and conduct problems as precursors to delinquency persistence in
boys: a comparison of three grade-based cohorts. Journal of Clinical Child and
Adolescent Psychology, 35, 46-59.
Paternite, C., & Loney, J.
(1980). Childhood hyperkinesis: Relationships between symptomatology and home
environment. In C. K. Whalen & B. Henker (Eds.), Hyperactive children: The
social ecology of identification and treatment (pp. 105-141). New York:
Academic Press.
Patterson, G. R. (1976). The
aggressive child: Victim and architect of a coercive system. In E. J. Mash, L.
A. Hamerlynck, & L. C. Handy (Eds.), Behavior modification and families
(pp. 267- 316). New York: Bruner/Mazel.
Patterson, G. R. (1982). Coercive
family process. Eugene, OR: Castalia.
Patterson, G. R., &
Chamberlain, P. (1994). A functional analysis of resistance during
parent-training therapy. Clinical Psychology: Science and Practice, 1, 53-70.
Patterson, G. R., Dishion, T. J.,
& Chamberlain, P. (1993). Outcomes and methodological issues relating to
treatment of antisocial children. In T. R. Giles (Ed.), Handbook of effective
psychotherapy. New York: Plenum Press.
Patterson, G. R., &
Fleischman, M. J. (1979). Maintenance of treatment effects: Some considerations
concerning family systems and follow-up data. Behavior Therapy, 10, 168-185.
Patterson, G. R., & Forgatch,
M. S. (1985). Therapist behavior as a determinant for client noncompliance: A
paradox for the behavior modifier. Journal of Consulting and Clinical
Psychology, 53, 846-851.
Patterson, G. R., Reid, J. B.,
& Dishion, T. J. (1992). Antisocial boys. Eugene, OR: Castalia.
Pearson, J. L., Ialongo, N. S.,
Hunter, A. G., & Kellam, S. G. (1993). Family structure and aggressive
behavior in a population of urban elementary school children. Journal of the
American Academy of Child and Adolescent Psychiatry, 33, 540-548.
Pelham, W. E., Jr., & Lang,
A. R. (1993). Parental alcohol consumption and deviant child behavior: Laboratory studies of reciprocal effects. Clinical Psychology Review, 13, 763–784.
Petty, C. R., Monuteaux, M. C.,
Mick, E., Hughes, S., Small, J., Faraone, S. V., & Biederman, J. (2009).
Parsing the familiality of oppositional defiant disorder from that of conduct
disorder: a family risk analysis. Journal of Psychiatric Research, 43,
345-352.
Pfiffner, L. J., Jouriles, E. N.,
Brown, M. M., Etscheidt, M. A., & Kelly, J. A. (1988, November). Enhancing
the effects of parent training for single-parent families. Paper presented at
the 22nd annual meeting of the Association for Advancement of Behavior Therapy,
New York.
Pfiffner, L. J., McBurnett, K.,
Rathouz, P. J., & Judice, S. (2005). Family correlates of oppositional and
conduct disorders in children with attention deficit/hyperactivity disorder.
Journal of Abnormal Child Psychology, 33, 551-563.
Pisterman, S., McGrath, P., Firestone,
P., Goodman, J. T., Webster, I., & Mallory, R. (1989). Outcome of
parent-mediated treatment of preschoolers with attention deficit disorder with
hyperactivity. Journal of Consulting and Clinical Psychology, 57, 628-635.
Pliszka, S. (2009). Treating
ADHD and Comorbid Disorders. New York: Guilford press.
Pollard, S., Ward, E., &
Barkley, R. (1983). The effects of parent training and Ritalin on the
parent-child interactions of hyperactive boys. Child and Family Behavior
Therapy, 5, 51-69.
Pressman, L. J., Loo, S. K.,
Carpenter, E. M., Asarnow, J. R., Lynn, D., McCracken, J. T., McGough, J. J.,
Lubke, G. H., Yang, M. H., & Smalley, S. L. (2006). Relationship of family
environment and parental psychiatric diagnosis to impairment in ADHD. Journal
of the American Academy of Child and Adolescent Psychiatry, 45, 346-354.
Prinz, R. J., & Miller, G. E.
(1994). Family-based treatment for childhood antisocial behavior: Experimental influences on dropout and engagement. Journal of Consulting and Clinical Psychology, 62, 645–650.
Prior, M. (1992). Childhood
temperament. Journal of Child Psychology and Psychiatry, 33, 249-279.
Psychogiou, L., Daley, D. M.,
Thompson, M. J., & Sonuga-Barke, E. J. S. (2008). Do maternal
attention-deficit/hyperactivity disorder symptoms exacerbate or ameliorate the
negative effect of child attention-deficit/hyperactivity disorder symptoms on
parenting? Development and Psychopathology, 20, 121-137.
Quici, F. L., Wheeler, S. R.,
& Bolle, J. (1996, March). Does training parents of defiant children really
work? Seven years of data. Paper presented at the annual meeting of the
National Association of School Psychologists, Atlanta, GA.
Rehabilitation Act of 1973, 29
U.S.C.A. § 701 et seq.
Reitman D., & McMahon, R. J.
(in press). Constance “Connie” Hanf (1917-2002): The mentor and the model.
Cognitive and Behavioral Practice.
Rejani, T. G., Oommen, A.,
Srinath, S., & Kapur, M. (2012). Efficacy of multimodal intervention for
children with attention deficit hyperactivity disorder (ADHD) - An Indian
study. Journal of Behavioral and Brain Sciences, 2, 117-127.
Reyno, S. M., & McGrath, P.
J. (2006). Predictors of parent training efficacy for child externalizing
behavior problems - a meta-analytic review. Journal of Child Psychology and
Psychiatry, 47, 99-111.
Reynolds, C., & Kamphaus, R.
(2015). Behavioral Assessment System for Children-III. Circle Pines, MN:
American Guidance Service.
Richters, J. E., & Cichetti,
D. (1993). Mark Twain meets DSM-III-R: Conduct disorder, development, and the
concept of harmful dysfunction. Development and Psychopathology, 5, 5-29.
Roberts, M. W., Hatzenbuehler, L.
C., & Bean, A. W. (1981). The effects of differential attention and time
out on child noncompliance. Behavior Therapy, 12, 93-99.
Roberts, M. W., McMahon, R. J.,
Forehand, R., & Humphreys, L. (1978). The effect of parental
instruction-giving on child compliance. Behavior Therapy, 9, 793-798.
Rogers, T. R., Forehand, R.,
Griest, D. L., Wells, K. C., & McMahon, R. J. (1981). Socioeconomic status:
Effects of parent and child behaviors and treatment outcome of parent training.
Journal of Clinical Child Psychology, 10, 98-101.
Roizen, N. J., Blondis, T. A.,
Irwin, M., & Stein, M. (1994). Adaptive functioning in children with
attention-deficit hyperactivity disorder. Archives of Pediatric and Adolescent
Medicine, 148, 1137-1142.
Rowe, R., Maughan, B., Pickles,
A., Costello, E. J., & Angold, A. (2002). The relationship between DSM-IV
oppositional defiant disorder and conduct disorder: findings from the Great Smoky
Mountains Study. Journal of Child Psychology and Psychiatry, 43, 365-373.
Russo, D. C., Cataldo, M. F.,
& Cushing, P. J. (1981). Compliance training and behavioral covariation in
the treatment of multiple behavior problems. Journal of Applied Behavior Analysis,
14, 209-222.
Rydell, A. M. (2010). Family
factors and children’s disruptive behavior: an investigation of links between demographic characteristics, negative life events and symptoms of ODD and ADHD. Social Psychiatry and Epidemiology, 45, 233-244.
Salzinger, S., Kaplan, S., &
Artemyeff, C. (1983). Mothers’ personal social networks and child maltreatment.
Journal of Abnormal Psychology, 92, 68-76.
Sanders, M. R. (1996). New
directions in behavioral family intervention with children. In T. H. Ollendick
& R. J. Prinz (Eds.), Advances in clinical child psychology (Vol. 18, pp.
283-330). New York: Plenum Press.
Sanders, M. R., &
Christensen, A. P. (1984). A comparison of the effects of child management and
planned activities training in five parenting environments. Journal of Abnormal
Child Psychology, 13, 101-117.
Sanders, M. R., & Dadds, M.
R. (1982). The effects of planned activities and child management procedures in
parent training: An analysis of setting generality. Behavior Therapy, 13,
452-461.
Sanders, M. R., & Glynn, T.
(1981). Training parents in behavioral self-management: An analysis of
generalization and maintenance. Journal of Applied Behavior Analysis, 14,
223-237.
Schachar, R., & Wachsmuth, R.
(1990). Oppositional Disorder in children: A validation study comparing Conduct
Disorder, Oppositional Disorder and normal control children. Journal of Child
Psychology and Psychiatry, 31, 1089-1102.
Schumaker, J. B., Hovell, M. F.,
& Sherman, J. A. (1977). An analysis of daily report cards and
parent-managed privileges in the improvement of adolescents’ classroom
performance. Journal of Applied Behavior Analysis, 10, 449-464.
Scott, S., & Dadds, M. R.
(2009). Practitioner review: when parent training doesn’t work: theory-driven
clinical strategies. Journal of Child Psychology and Psychiatry, 50,
1441-1450.
Seeley, J. R., Small, J. W.,
Walker, H. M., Fell, E. G., Severson, H. H., Golly, A. M., & Forness, S. R.
(2009). Efficacy of the First Step to Success intervention for students with attention-deficit/hyperactivity
disorder. School mental Health, 1, 37-48.
Shaw, D. S., & Vondra, J. I.
(1995). Infant attachment security and maternal predictors of early behavior
problems: A longitudinal study of low-income families. Journal of Abnormal Child
Psychology, 23, 335-357.
Shelton, T. L., Barkley, R. A.,
Crosswait, C., Moorehouse, M., Fletcher, K., Barrett S., Jenkins, L., &
Metevia, L. (1998). Psychiatric and psychological morbidity as a function of
adaptive disability in preschool children with aggressive and
hyperactive-impulsive-inattentive behavior. Journal of Abnormal Child
Psychology, 26, 475-494.
Shriver, M. D., & Allen, K.
D. (1996). The time-out grid: A guide to effective discipline. School
Psychology Quarterly, 11, 67-75.
Singh, A. L., & Waldman, I.
D. (2010). The etiology of associations between negative emotionality and
childhood externalizing disorders. Journal of Abnormal Psychology, 119,
376-388.
Snyder, J., & Brown, K.
(1983). Oppositional behavior and noncompliance in preschool children:
Environmental correlates and skills deficits. Behavioral Assessment, 5,
333-348.
Snyder J., & Patterson, G. R.
(1995). Individual differences in social aggression: A test of the
reinforcement model of socialization in the natural environment. Behavior
Therapy, 26, 371-391.
Sonuga-Barke, E.J.S., Daley, D.,
& Thompson, M. (2002). Does maternal ADHD reduce the effectiveness of
parent training for preschool children’s ADHD? Journal of the American Academy
of Child and Adolescent Psychiatry, 41, 696-702.
Spaccarelli, S., Cotler, S.,
& Penman, D. (1992). Problem-solving skills training as a supplement to
behavioral parent training. Cognitive Therapy and Research, 16, 1-18.
Sparrow, S. S., Cicchetti, D. V.,
& Balla, D. A. (2005). Vineland Adaptive Behavior Scales (2nd ed.). Circle Pines, MN: American Guidance Service.
Speltz, M. L., McClellan, J.,
DeKlyen, M., & Jones, K. (1999). Preschool boys with oppositional defiant
disorder: clinical presentation and diagnostic change. Journal of the
American Academy of Child and Adolescent Psychiatry,36, 635-645.
Speltz, M. L., DeKlyen, M.,
Greenberg, M. T., & Dryden, M. (1995). Clinic referral for oppositional
defiant disorder: Relative significance of attachment and behavioral variables.
Journal of Abnormal Child Psychology, 23, 487-507.
Spitzer, A., Webster-Stratton,
C., & Hollinsworth, T. (1991). Coping with conduct-problem children:
Parents gaining knowledge and control. Journal of Clinical Child Psychology, 20,
413-427.
Stadler, C., Grasmann, D.,
Fegert, J. M., Holtmann, M., Poustka, F., & Schmeck, K. (2008). Heart rate
and treatment effect in children with disruptive behavior disorders. Child
Psychiatry and Human Development, 39, 299-309.
Steinhausen, H.C., Gollner, J.,
Brandeis, D., Muller, U. C., Valko, L., & Drechsler, R. (2012).
Psychopathology and personality in parents of children with ADHD. Journal of
Attention Disorders, online first, DOI: 10.1177/1087054711427562.
Stingaris, A. & Goodman, R.
(2009). Longitudinal outcome of youth oppositionality: irritable, headstrong,
and hurtful behaviors have distinctive predictions. Journal of the
American Academy of Child and Adolescent Psychiatry,48, 404-412.
Stingaris, A., Maughan, B., &
Goodman, R. (in press). What’s in a disruptive disorder? Temperamental
antecedents of oppositional defiant disorder: findings from the Avon
longitudinal study. Journal
of the American Academy of Child and Adolescent Psychiatry.
Stormont-Spurgin, M., &
Zentall, S. S. (1995). Contributing factors in the manifestation of aggression
in preschoolers with hyperactivity. Journal of Child Psychology and Psychiatry,
3, 491-509.
Strain, P. S., Steele, P., Ellis,
T., & Timm, M. A. (l982). Long-term effects of oppositional child treatment
with mothers as therapists and therapist trainers. Journal of Applied Behavior
Analysis, 15, 163-169.
Strain, P. S., Young, C. C.,
& Horowitz, J. (1981). Generalized behavior change during oppositional
child training: An examination of child and family demographic variables. Behavior
Modification, 5, 15-26.
Strayhorn, J. M., & Weidman,
C. S. (1989). Reduction of attention deficit and internalizing symptoms in
preschoolers through parent-child interaction training. Journal of the American
Academy of Child and Adolescent Psychiatry, 28, 888-896.
Strayhorn, J. M., & Weidman,
C. S. (1991). Follow-up one year after parent-child interaction training:
Effects on behavior of preschool children. Journal of the American Academy of
Child and Adolescent Psychiatry, 30, 138-143.
Thapar, A. & Goozen, S. van (2018). Conduct disorder in ADHD. In Banaschewski, T., Coghill, D., & Zuddas, A. (eds.). Oxford Textbook of Attention Deficit Hyperactivity Disorder (pp. 193-199). London: Oxford University Press.
Theule, J., Wiener, J., Rogers, M.
A., & Marton, I. (2011). Predicting parenting stress in families of
children with ADHD: parenting and contextual factors. Journal of Child and
Family Studies, 20, 640-647.
Thomas, R., & Zimmer-Gembeck,
M. J. (2007). Behavioral outcomes of Parent-Child Interaction Therapy and
Triple P – Positive Parenting Program: a review and meta-analysis. Journal of
Abnormal Child Psychology, 35, 475-495.
Thompson, M. J. J.,
Laver-Bradbury, C., Ayres, M., Poidevin, E. L., Mead, S., Dodds, C.,
Psychogiou, L., Bitsakou, P., Daley, D., Weeks, A., Brotman, L. M., Abikoff,
H., Thompson, P., & Sonuga-Barke, E. J. S. (2009). A small-scale
randomized controlled trial of the revised new forest parenting programme for
preschoolers with attention deficit hyperactivity disorder. European Child and
Adolescent Psychiatry, 18, 605-616.
Tremblay, R. E., Masse, B.,
Perron, D., Leblanc, M., Schwartzman, A. E., & Ledingham, J. E. (1992).
Early disruptive behavior, poor school achievement, delinquent behavior, and
delinquent personality: Longitudinal analyses. Journal of Consulting and
Clinical Psychology, 60, 65-72.
Tremblay, R. E., Pihl, R. O.,
Vitaro, F., & Dobkin, P. L. (1994). Predicting early onset of male
antisocial behavior from preschool behavior. Archives of General Psychiatry, 51,
732-738.
Tschann, J. M., Kaiser, P.,
Chesney, M. A., Alkon, A., & Boyce, W. T. (1996). Resilience and
vulnerability among preschool children: Family functioning, temperament, and
behavior problems. Journal of the American Academy of Child and Adolescent
Psychiatry, 35, 184-191.
Tully, E. C., Iacono, W. G.,
& McGue, M. (2008). An adoption study of parental depression as an
environmental liability for adolescent depression and childhood disruptive
disorders. American Journal of Psychiatry, 165, 1148-1154.
Tuvblad, C., Zheng, M., Raine,
A., & Baker, L. A. (2009). A common genetic factor explains the
covariation among ADHD, ODD, & CD symptoms in 9-10 year old boys and
girls. Journal of Abnormal Child Psychology, 37, 153-167.
Vaden-Kiernan, N., Ialongo, N.
S., Pearson, J., & Kellam, S. (1995). Household family structure and
children’s aggressive behavior: A longitudinal study of urban elementary school children. Journal of Abnormal Child Psychology, 23, 553–568.
Vuchinich, S., Bank, L., &
Patterson, G. R. (1992). Parenting, peers, and the stability of antisocial
behavior in preadolescent boys. Developmental Psychology, 28, 510-521.
Wagern, S. M., & McNeil, C.
B. (2008). Parent-Child Interaction Therapy for ADHD: a conceptual overview
and critical literature review. Child and Family Behavior Therapy, 30,
231-256.
Wahler, R. (1975). Some
structural aspects of deviant child behavior. Journal of Applied Behavior
Analysis, 8, 27-42.
Wahler, R. G. (1980). The insular
mother: Her problems in parent-child treatment. Journal of Applied Behavior
Analysis, 13, 207-219.
Wahler, R. G., & Afton, A. D.
(1980). Attentional processes in insular and noninsular mothers: Some
differences in their summary reports about child problem behaviors. Child
Behavior Therapy, 2, 25-41.
Wahler, R. G., Cartor, P. G.,
Fleischman, J., & Lambert, W. (1993). The impact of synthesis teaching and
parent training with mothers of conduct-disordered children. Journal of
Abnormal Child Psychology, 21, 425-440.
Wahler, R. G., & Fox, J. J.
(1980). Solitary toy play and time out: A family treatment package for children
with aggressive and oppositional behavior. Journal of Applied Behavior Analysis,
13, 23-39.
Wahler, R. G., & Graves, M.
G. (1983). Setting events in social networks: Ally or enemy in child behavior
therapy? Behavior Therapy, 14, 19-36.
Waldman, I. D., Rowe, R., Boylan, K., & Burke, J. D. (2021). External validation of a bifactor model of oppositional defiant disorder. Molecular psychiatry, 26, 682-693.
Wakefield, J. C. (1992). Disorder
as harmful dysfunction: A conceptual critique of DSM-III-R’s definition of
mental disorder. Psychological Review, 99, 232-247.
Waschbusch, D. A., Carrey, N. J.,
Willoughby, M. T., King, S., & Andrade, B. F. (2007). Effects of
methylphenidate and behavior modification on the social and academic behavior
of children with disruptive behavior disorders: The moderating role of
callous/unemotional traits. Journal of Clinical Child and Adolescent
Psychology, 36, 629-644.
Webster-Stratton, C. (1982). The
long-term effects of a videotape modeling parent-training program: Comparison
of immediate and 1-year follow-up results. Behavior Therapy, 13, 702-714.
Webster-Stratton, C. (1984).
Randomized trial of two parent-training programs for families with conduct
disordered children. Journal of Consulting and Clinical Psychology, 52,
666-678.
Webster-Stratton, C. (1991).
Stress: A potential disruptor of parent perceptions and family interactions. Journal
of Clinical Child Psychology, 19, 302-312.
Webster-Stratton, C. (2006). Incredible Years Parenting Program. Seattle, WA: Incredible Years.
Webster-Stratton, C., &
Hammond, M. (1990). Predictors of treatment outcome in parent training for families
with conduct problem children. Behavior Therapy, 21, 319-337.
Webster-Stratton, C.,
Hollinsworth, T., & Kolpacoff, M. (1989). The long-term effectiveness and
clinical significance of three cost-effective training programs for families
with conduct-problem children. Journal of Consulting and Clinical Psychology, 57,
550-553.
Webster-Stratton, C., Kolpacoff,
M., & Hollinsworth, T. (1995). Self-administered videotape therapy for
families with conduct-problem children: Comparison with two cost-effective
treatments and a control group. Journal of Consulting and Clinical Psychology, 56,
558-566.
Webster-Stratton, C., &
Spitzer, A. (1996). Parenting a young child with conduct problems. In T. H.
Ollendick & R. J. Prinz (Eds.), Advances in clinical child psychology (Vol.
18, pp. 1-62). New York: Plenum Press.
Wells, K. C., & Forehand, R.
(1985). Conduct and Oppositional Disorders. In P. H. Bornstein & A. E.
Kazdin (Eds.), Handbook of clinical behavior therapy with children (pp.
219-265). Champaign, IL: Dorsey Press.
Wells, K. C., Forehand, R., &
Griest, D. L. (1980). Generality of treatment effects from treated to untreated
behaviors resulting from a parent training program. Journal of Clinical Child
Psychology, 9, 217-219.
Wenning, K., Nathan, P., &
King, S. (1993). Mood disorders in children with oppositional defiant disorder:
A pilot study. American Journal of Orthopsychiatry, 63, 295-299.
Whittinger, N. S., Langley, K.,
Fowler, T. A., Thomas, H. V., & Thapar, A. (2007). Clinical precursors of
adolescent conduct disorder in children with attention-deficit/hyperactivity
disorder. Journal of the American Academy of Child and Adolescent Psychiatry, 46,
179-187.
Wilens, T. (2008). Straight talk
about psychiatric medications for children (2nd ed.). New York:
Guilford Press.
Williams, C. A., & Forehand,
R. (1984). An examination of predictor variables for child compliance and
noncompliance. Journal of Abnormal Child Psychology, 12, 491-504.
Wood, A. C., Rijsdijk, F.,
Asherson, P., & Kuntsi, J. (2009). Hyperactive-impulsive symptom scores
and oppositional behaviours reflect alternate manifestations of a single liability.
Behavior Genetics, 39, 447-460.
Worland, J., Carney, R., Milich,
R., & Grame, C. (1980). Does in-home training add to the effectiveness of
operant group parent training? Child Behavior Therapy, 2, 11-24.
Wymbs, B. T., Pelham, W. E. Jr.,
Molina, B. S. G., Gnagy, E. M., Wilson, T. K., & Greenhouse, J. B. (2008).
Rate and predictors of divorce among parents of youth with ADHD. Journal of
Consulting and Clinical Psychology, 76, 735-744.
Zoccolillo, M. (1993). Gender and
the development of conduct disorder. Development and Psychopathology, 5, 65-78.


 ContinuingEdCourses.Net is approved by the American Psychological Association (APA) to sponsor continuing education for psychologists. ContinuingEdCourses.Net maintains responsibility for this program and its content.
ContinuingEdCourses.Net is approved by the American Psychological Association (APA) to sponsor continuing education for psychologists. ContinuingEdCourses.Net maintains responsibility for this program and its content. ContinuingEdCourses.Net, provider #1107, is approved as an ACE provider to offer social work continuing education by the Association of Social Work Boards (ASWB) Approved Continuing Education (ACE) program. Regulatory boards are the final authority on courses accepted for continuing education credit. ACE provider approval period: 3/9/2005-3/9/2027.
ContinuingEdCourses.Net, provider #1107, is approved as an ACE provider to offer social work continuing education by the Association of Social Work Boards (ASWB) Approved Continuing Education (ACE) program. Regulatory boards are the final authority on courses accepted for continuing education credit. ACE provider approval period: 3/9/2005-3/9/2027. ContinuingEdCourses.Net has been approved by the National Board for Certified Counselors (NBCC) as an Approved Continuing Education Provider (ACEP), ACEP #6323. Programs that do not qualify for NBCC credit are clearly identified. ContinuingEdCourses.Net is solely responsible for all aspects of the programs.
ContinuingEdCourses.Net has been approved by the National Board for Certified Counselors (NBCC) as an Approved Continuing Education Provider (ACEP), ACEP #6323. Programs that do not qualify for NBCC credit are clearly identified. ContinuingEdCourses.Net is solely responsible for all aspects of the programs. ContinuingEdCourses.Net is recognized by the New York State Education Department's State Board for Psychology (NYSED-PSY) as an approved provider of continuing education for licensed psychologists #PSY-0048.
ContinuingEdCourses.Net is recognized by the New York State Education Department's State Board for Psychology (NYSED-PSY) as an approved provider of continuing education for licensed psychologists #PSY-0048.




